855 DOI: 10.1590/0004-282X20160110
ARTICLE HISTORICAL NOTE
A tribute to Wartenberg’s refined neurological
examination
Um tributo ao refinado exame neurológico de Wartenberg
Péricles Maranhão-Filho1, Renato Gonik2
Robert Wartenberg was born in 1887 in Grodno, Belarus, then part of the Russian Empire1. He received his medical
degree from the University of Rostock, Germany, in 1919, and was, for many years, associated with the University of Freiburg, where he became Professor of Neurology in 19332.
With the Nazi regime in power, rising anti-Semitism led him
to lee Germany in 1935. After relocating to the United States
in 1936, he re-engaged in his neurology career at the University of California Medical School in San Francisco, where he was
appointed Clinical Professor of Neurology in 19522.
Wartenberg was an internationally recognized neurologist, earning an honorary membership in several foreign societies. Of
note, in 1953, the California Medicine Journal3 published the
fol-lowing announcement: “Dr. Robert Wartenberg, clinical professor of neurology, University of California Hospital, has been elected a corresponding member of the Rio de Janeiro Society of Neurology”.
Wartenberg’s academic accomplishments were vast. He believed in a “sacred obligation” to his students, and report-edly his lectures were unforgettable events1. Wartenberg
made over 150 scientiic contributions, including four
books1: he Examination of Relexes: A Simpliication (1945)4;
Hemifacial Spasm (1952)5; Diagnostic Tests in Neurology
(1953)6; and Neuritis, Sensory Neuritis, Neuralgia (1958)7.
He was reputed to be one of the foremost semiologists of his time. He strived to abolish unnecessary eponym designations,
leading an efort to replace them with designations that were
descriptive of the underlying pathophysiology8. In fact, he was
known to be very critical of the neurological literature, some-what intolerant of carelessness, albeit with a constructive intent. We pay homage to Wartenberg’s tradition of
simplify-ing the examination by briely discusssimplify-ing ive of his seminal
neurological signs.
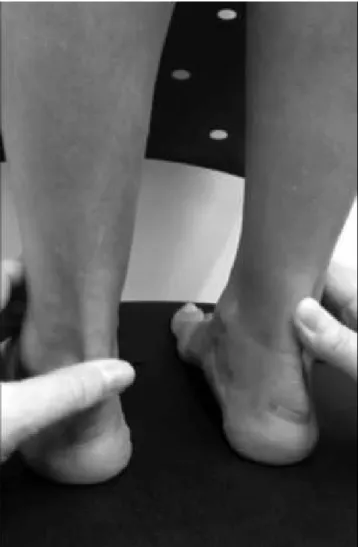
TENDON PALPATION TEST
A lesion of the lower motor neurons lead to muscle hypoto
-nia, resulting in tendon slackness. his is best seen in the Achilles
tendon. With the patient standing upright, weight equally dis-tributed onto both legs, the examiner gently grasps the patient’s
ankles, placing his thumbs directly over the Achilles tendons.
Pressure is gradually exerted over each tendon, while comparing
the resistance ofered against the thumbs (Figure 1).
In a normal person standing lat onto his feet, the Achilles
tendon has a hard consistency. In unilateral lesions of the
sci-atic nerve the Achilles tendon has a softer consistency when
compared to the normal side.
his sensitive test may indicate the presence of a lower motor
neuropathy at a very early stage when no evidence of muscle
wasting, weakness, or even diminished ankle jerk is present. A soft
1Universidade Federal do Rio de Janeiro, Faculdade de Medicina, Serviço de Neurologia, Hospital Universitário Clementino Fraga Filho, Rio de Janeiro RJ, Brasil;
2Director, Clinical Neurophysiology Consultants, Hollywood, FL.
Correspondence: Péricles Maranhão-Filho; Rua Prefeito Dulcídio Cardoso, 1680/1802; 22260-311 Rio de Janeiro RJ, Brasil; E-mail: [email protected] Conflict of interest: There is no conlict of interest to declare.
Received 22 March 2016; Accepted 06 June 2016.
ABSTRACT
Robert Wartenberg was a renowned 20th century neurologist who contributed greatly to our understanding of the neurological examination. This article aims to illustrate his legacy by highlighting ive seminal neurological signs.
Keywords: Robert Wartenberg; neurologic examination.
RESUMO
Robert Wartenberg foi um renomado neurologista do século XX que contribuíu enormemente para o entendimento do exame neurológico. Este artigo tem como objetivo principal ilustrar seu legado, ressaltando cinco sinais neurológicos seminais.
856 Arq Neuropsiquiatr 2016;74(10):855-857
Achilles tendon may thus be an early sign of sciatic neuropathy.
When positive, this test corroborates an organic peripheral lesion of the nervous system, but a negative test cannot exclude it6.
LID VIBRATION TEST
he seemingly smooth process of sustained voluntary
muscle contraction is a result of the continuous integration of
multiple underlying discrete and successive contractions. his ine-tuning mechanism is evident in the orbicularis oculi as a
palpable vibratory sensation that declines with weakness. It can be felt by applying gentle lateral traction at the outer canthus
while the patient maintains forceful eyelid closure (Figure 2).
Diminished lid vibration is a very sensitive sign, occurring early in cases of slowly evolving facial palsy. Conversely, its return to normality occurs slowly and late in the process of recovery. In fact, it may remain diminished as a sole indication of an old
facial palsy. As such, diminished lid vibration may be the irst, as
well as last, sign detected in the natural history of a facial palsy.
Despite its sensitivity, it is not speciic in distinguishing central
from peripheral facial lesions, being present in both6.
ASSOCIATED MOVEMENT OF THE THUMB
Volitional hand movements require precise control of
agonist, antagonist, and synergist muscles. his orchestra -tion is compromised by lesions of central descending motor pathways, resulting in unusual patterns of motor activation. One such pattern is observed in the spastic paretic hand as an associated movement of the thumb.
he patient is asked to pull his four ingers, lexed at the terminal phalanges, against resistance ofered by the exam
-iner’s similarly lexed ingers (Figure 3).
In a normal person, the thumb remains extended and abducted. Conversely, spastic paresis of the hand results in
involuntary thumb adduction, lexion, and opposition. his
constitutes a very early sign, and may be seen in incipient spastic hand paresis6.
WRIST DROP TEST
Weakness of wrist extension results in a hand droop when
the patient’s pronated forearm is held horizontally, and ingers are relaxed. Inspection alone cannot diferentiate if this phenom -enon is due to a central or peripheral lesion. However, clenching
the ingers while the hand is in this position can make this dis -tinction6 (Figure 4). Normally, lexion of the ingers is accompa
-nied by extension at the wrist as an associated movement. his motor response is preserved with lesions afecting central motor
pathways, and is lost with peripheral lesions.
he patient is asked to grasp an object with his afected hand. With peripheral lesions afecting the extensor musculature, such as a radial neuropathy, dorsilexion is absent. In fact, wrist lexion may be accentuated by increasing efort to tighten the grip. With central lesions, wrist dorsilexion occurs involuntarily.
ACCESSORY NERVE TEST
he spinal accessory nerve innervates the upper trape
-zius muscle, which acts to elevate the shoulder. his thin nerve lies supericially and is easily traumatized, often an iat -rogenic lesion of the posterior triangle of the neck9.
857
Maranhão-Filho P, Gonik R. Wartenberg’s neurological examination
In the event of an accessory nerve lesion a shoulder droop
occurs. his displacement results in an apparent length dis
-crepancy of the upper limbs. he patient is examined upright with arms hanging loosely at the sides. he level at which the ingertips touch the thighs are compared. On the afected side the ingertips touch the thigh at a lower level than on the healthy side (Figure 5).
Robert Wartenberg was a respected igure in the global
neurological community, in great measure due to his didactic acumen2. In today’s overly technological environment,
remem-bering Wartenberg’s signs may rekindle the art of examination.
Figure 3. Associated movement of the thumb. In mild spastic
paresis the thumb moves toward the palm. The examiner is wearing a wristwatch.
Figure 5. Accessory nerve test. Fingertips on affected side
(right) extend below the level on healthy side (black line).
Figure 4. Wrist drop (A). In laccid paresis wrist lexion is exacerbated (B). In spastic paresis involuntary wrist extension occurs (C).
A
B
C
References
1. Aird RB. Robert Wartenberg, MFF., 1887−1956. Neurology. 1957;7(2):146-47. doi:10. 1212/ WNL. 7. 2. 146
2. Lange O. Homenagem póstuma: Prof. Robert Wartenberg. Arq Neuropsiquiatr. 1957;15(1):91-2. doi:10.1590/S0004-282X1957000100010
3. News & Notes. California Medicine. 1953;78(4):332-3.
4. Wartenberg R. The examination of relex a simpliication. Chicago: The Year Book; 1945.
5. Wartenberg R. Hemifacial spasm. New York: Oxford University Press; 1952.
6. Wartenberg R. Diagnostic test in neurology. Chicago: The Year Book; 1953.
7. Wartenberg R. Neuritis, sensory neuritis, neuralgia. New York: Oxford University Press; 1958.
8. Wartenberg R. On neurologic terminology, eponyms and the Lasègue sign. Neurology. 1956;6(12):853-8. doi: 10. 1212/ WNL. 6. 12. 853