w w w . r b h h . o r g
Revista
Brasileira
de
Hematologia
e
Hemoterapia
Brazilian
Journal
of
Hematology
and
Hemotherapy
Original
article
Dangerous
universal
donors:
the
reality
of
the
Hemocentro
in
Belo
Horizonte,
Minas
Gerais
Mariana
Martins
Godin
a,b,
Lucas
de
Oliveira
Souza
b,
Luciana
Cayres
Schmidt
b,
Lauro
Mello
Vieira
a,
Rejane
Silva
Diniz
a,
Luci
Maria
SantAna
Dusse
a,∗aUniversidadeFederaldeMinasGerais(UFMG),BeloHorizonte,MG,Brazil
bFundac¸ãoCentraldeImuno-Hematologia,Fundac¸ãoHemominas,BeloHorizonte,MG,Brazil
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received16October2015 Accepted18May2016 Availableonline16June2016
Keywords:
Hemagglutinins IgM
IgG
Dangerousuniversaldonor Hemolytictransfusionreaction
a
b
s
t
r
a
c
t
Background:Thetermdangerousuniversalblooddonorreferstopotentialagglutinationof theerythrocytesofnon-OrecipientsduetoplasmaofanObloodgroupdonor,which con-tainshightitersofanti-Aand/oranti-Bhemagglutinins.Thus,priortitrationofanti-Aand anti-Bhemagglutininsisrecommendedtopreventtransfusionreactions.
Objective:Theaimofthisstudywastoestimatethefrequencyofdangerousuniversaldonors inthebloodbankofBeloHorizonte(Fundac¸ãoCentraldeImuno-Hematologia–Fundac¸ão Hemominas–MinasGerais)bydeterminingthetitersofanti-Aandanti-Bhemagglutinins inObloodgroupdonors.
Method:Atotalof400Obloodgroupdonorswererandomlyselected,fromMarch2014to Jan-uary2015.Thetitersofanti-Aandanti-Bhemagglutinins(IgMandIgGclasses)wereobtained usingthetubetitrationtechnique.Dangerousdonorswerethosewhosetitersofanti-Aor anti-BIgMwere≥128and/orthetitersofanti-Aoranti-BIgGwere≥256.Donorswere
char-acterizedaccordingtogender,ageandethnicity.Thehemagglutininswerecharacterizedby specificity(anti-Aandanti-B)andantibodyclass(IgGandIgM).
Results:Almostone-third(30.5%)oftheObloodgroupdonorswereuniversaldangerous. Thefrequencyamongwomenwashigherthanthatofmen(p-value=0.019;oddsratio:1.66; 95%confidenceinterval:1.08–2.56)andamongyoungdonors(18–29yearsold)itwashigher thanfordonorsbetween49and59yearsold(p-value=0.015;oddsratio:3.05;95% confi-denceinterval:1.22–7.69).Therewasnosignificantassociationbetweendangerousuniversal donorsandethnicity,agglutininspecificityorantibodyclass.
Conclusion: Especiallyplateletconcentratesobtainedbyapheresis(thatcontaina substan-tialvolumeofplasma),comingfromdangerousuniversaldonorsshouldbetransfusedin isogrouprecipientswheneverpossibleinordertopreventtheoccurrenceoftransfusion reactions.
©2016Associac¸ ˜aoBrasileiradeHematologia,HemoterapiaeTerapiaCelular.Published byElsevierEditoraLtda.ThisisanopenaccessarticleundertheCCBY-NC-NDlicense (http://creativecommons.org/licenses/by-nc-nd/4.0/).
∗ Correspondingauthorat:FaculdadedeFarmácia, UniversidadeFederaldeMinasGerais(UFMG),Av.AntônioCarlos,6627,Campus
Pampulha,31270-901BeloHorizonte,MG,Brazil. E-mailaddress:[email protected](L.M.Dusse).
http://dx.doi.org/10.1016/j.bjhh.2016.05.007
Introduction
Knowledge about the ABO system, from the first exper-iments of Karl Landsteiner established the beginning of scientifictransfusion medicine.1 Ottenberg gaveapriceless
contribution tostart the practiceoftransfusions,when he demonstrated that the occurrence oftransfusion reactions dependon,amongotherfactors,thetitersofhemagglutinins indonorplasma.2
It is known that anti-A and anti-B hemagglutinins are potentIgMandIgGantibodiesthatbindtoantigensAandBon thesurfaceoferythrocytesandmayactivatethecomplement cascaderesultinginacuteintravascularhemolysis.3The
anti-gensoftheABOsystemareexpressedinerythroidprecursors fromthefifthorsixthweekofintrauterinelife.Themaximum expressionoftheseantigensisobtainedbetweentwoandfour yearsold.4
The term dangerous universal blood donor was first described in 1923 in reference to the agglutination poten-tialoferythrocytesofnon-Orecipients,duetoplasmaofO bloodgroupdonorsthatcontainshightitersofanti-Aoranti-B hemagglutinins.5Intheclinicalpractice,theterm‘dangerous’
referstotheinvivohemolyticpotentialofhightitersof hemag-glutininspresentintheplasmaofObloodgroupdonors.Thus, priortitrationofanti-Aandanti-Bhemagglutininsis recom-mendedtopreventtransfusionreactions.
Theaimofthisstudy was toestimatethe frequencyof dangerousuniversaldonorsintheblood bankofBelo Hori-zonte(Fundac¸ão Centrode HematologiaeHemoterapia de MinasGerais–Hemominas)bydeterminingtitersofanti-A andanti-BhemagglutininsinO bloodgroupdonorsand to proposemeasurestopreventiatrogeniccomplications.
Method
Studydesign
This study was approved by the local Ethics Committees (Fundac¸ãoHemominasandtheUniversidadeFederaldeMinas Gerais)andwasconductedintheImmunohematologyCenter ofthebloodbankinBeloHorizonte.
Thesamplecalculationwasmadeconsideringthe num-berofObloodgroupdonorsinthebloodbankin2012(34,647 donors),theprevalenceofdangerousuniversaldonorsin sim-ilarstudiesconductedinBrazil(averageapproximately10%) andalevelofsignificanceof5%.Thiscalculationindicated theneed toanalyzeatleast400samplesofO bloodgroup donors to estimate the frequency of dangerous universal donors.6
O blood group donors were selected randomly, accord-ing tothe following inclusion criteria: absence ofirregular antibodyscreeningand negativehemoglobinS test results regardlessoftheRhDphenotype,ethnicity,ageandgender. Exclusion criteriawere Oblood groupdonorsthathad any positive testresults mentioned aboveand those with A, B orAB bloodgroupsand subgroups.Samplesobtainedfrom O blood group donors were evaluated from March 2014 to January2015.
Hemagglutinintitrationtechnique
Thetitersofanti-Aandanti-Bhemagglutininswereperformed usingthetubetechnique,whichisconsideredstandard.7
The titration of anti-A and anti-B hemagglutinins (IgM class)wasperformedbyserialdilutionsofdonorplasma col-lectedinethylenediaminetetraaceticacid(EDTA)usingsaline solution (from 1:1until1:1024).Thelast tube waskeptfor furtherdilutionsifnecessary.
Then,5%suspensionsofredbloodcells(A1and B)were
added,givingafinalvolumeof100L.Thetubeswere
incu-bated for 15min atroom temperature and centrifuged for reading,inaccordancewiththelaboratory’snorms(1000rpm foroneminute).Anagglutinationreadingwasperformedfor eachtube.Thetiterwasdefinedastheinverseofthelast dilu-tionthatproducedanequivalentof1+agglutination.Thisis characterizedbyaslightlyagglutinatedblurredbackgroundas describedintheTechnicalManualoftheAmerican Associa-tionofBloodBank(AABB).8Whenthetitersofanti-Aoranti-B
hemagglutininswere≥128,donorswereconsideredtobein
thedangerousuniversalgroup.9
Forthetitrationofanti-Aandanti-Bhemagglutinins(IgG class),thedonorplasmawastreatedwith0.01Mdithiothreitol (DTT–Sigma–Aldrich®)todestroyIgMclass
immunoglobu-lins,sothattheywouldnotinterferewiththequantification ofIgGclasshemagglutinins.Then,serialdilutionswere pre-pared withthe treatedplasma insaline solution [from1:2 (DTT+plasma)until1:1024].Thelast tubewaskeptfor fur-therdilutionsifnecessary.Then,5%suspensionsofredblood cells(A1andB)wereadded,givingafinalvolumeof100L.
Thetubeswereincubatedfor15minat37◦Candthe
erythro-cyteswerewashedthreetimeswithsalinesolution.Coombs monospecific IgG anti-serum (Lorne®) was added and the
tubeswerecentrifugedforreadinginaccordancewiththe lab-oratory’snorms(1000rpmforoneminute).Anagglutination readingwasperformedforeachtube.Thetiterwasdefined as theinverse ofthe last dilutionthat producedan equiv-alentof1+agglutination.Thisischaracterizedbyaslightly agglutinatedblurredbackgroundasdescribedbythe Techni-calManualoftheAABB.8Whenthetitersofanti-Aoranti-B
hemagglutininswere≥256,donorswereconsideredtobein
thedangerousuniversalgroup.10
Statistical analysis was performed using the GraphPad Prism(version5.0)andMinitab(17thversion)software.A cal-culation ofthe number ofsamplesclassified asdangerous was performed with the result expressed as a percentage of O blood group donors. The analyses of the association betweenhemagglutinintitersandgender,ethnicityandage usedthechi-squaretest(2).Whentheexpectedvalueswere ≤5,Fisher’sexacttestwasusedtoverifyassociations.p-Values ≤0.05wereconsideredsignificant.
Oddsratio(OR)and95%confidenceintervals(95%CI)were determinedforthevariablesthatshowedanyassociationwith thehemagglutinintiters.
Results
Not dangerous 69.5% (278)
Dangerous 30.5% (122)
Figure1–RelativefrequencyofObloodgroupdonors
classifiedasdangerousandnon-dangerous.
tothesetcut-offpoints,regardlessoftheantibodyclass.In 278samples(69.5%),theanti-Aoranti-Bhemagglutinintiters werelowerthanthecut-offpoint(Figure1).
Ofthe400samplesevaluated,209werefrommen(52.3%) and 191were from women(47.7%). Ofthemen, 53 (25.3%) wereclassifiedasdangerousuniversaldonorsand156(74.7%) as non-dangerous. Of the women, 69 (36.1%) were classi-fiedasdangerousdonorsand122(63.9%)asnon-dangerous. Accordingtothechi-squaretest, thepercentageof danger-ousuniversaldonorswassignificantlyhigheramongwomen (p-value=0.019)(Figure2).
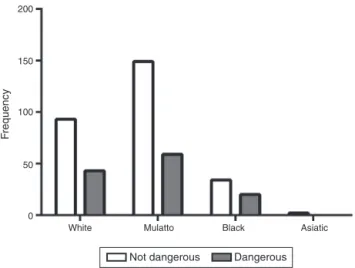
Regardingethnicity,ofthe400donorsincludedinthe sur-vey, 136 declared themselves as White (34%), 54 as Black (13.5%),208asMulatto(52%)andtwoasAsiatic(0.5%).Ofthe 122donorsclassifiedasdangerous,43(35.2%)declared them-selvesasWhite,20(16.4%)asBlackand59(48.4%)asMulatto. Onapplyingthechi-squareandFisher’sexacttests,therewas noassociation betweentheethnicalbackground andbeing classifiedasadangerousdonor(Figure3).
Regardingtheagegroup,ofthe400donorsincludedinthis survey,169(42.2%)donorswerebetween18and28yearsold, 116(29.0%)werefrom29to38yearsold,69(17.3%)from39 to48years old,36(9.0%)between49 and58 yearsold and 10 (2.5%) were from 59 to 69 years old.Of the 122 donors
200
150
100
50
0
Men
F
requency
Women
Not dangerous Dangerous
*
*
Figure2–Absolutefrequenciesofdonorsstratifiedby
genderandclassifiedasdangerousornon-dangerous.
*Significantdifferencebetweengroups(p-value<0.05).
200
150
100
50
0
F
requency
Not dangerous
White Mulatto Black Asiatic
Dangerous
Figure3–Absolutefrequenciesofevaluateddonors
stratifiedbyethnicityandclassifiedasdangerousor
non-dangerous.
classified as dangerous, 64 (52.4%) belonged to the 18–28 year-old age group,32 (26.2%) tothe 29–38year-old group, 18 (14.8%) to the 39–48 year-old group, six (5.0%) to the 49–58 year-old group and two (1.6%) to the 59–69 year-old group.Onapplyingthechi-squaretest,therewereno signif-icantdifferencesexceptinrespecttothe18–28year-oldand 49–58years-oldgroups(p-value=0.015).Forthe59–69year-old group,statisticalanalysisusedtheFisher’sexacttestandthere werenosignificantdifferencescomparedtotheothergroups (Figure4).
Regarding the specificity of hemagglutinins (Table 1), univariateanalysisofthedatarevealednosignificant asso-ciation between being classified as a dangerous universal donor and higher anti-A or anti-Bhemagglutinin titers (p -value=0.7468).
Inrespecttotheantibodyclass(Table2),univariate analy-sisshowednosignificantassociationbetweenbeingclassified asadangerousuniversaldonorandhigherIgMorIgGclass antibodytiters(p-value=0.4846).
150
100
50
*
*
0
18-28 29-38 39-48 49-58 59-69
F
requency
Not dangerous Dangerous
Figure4–Absolutefrequencyofdonorsstratifiedbyage
andclassifiedasdangerousornon-dangerous.*Significant
Table1–Distributionofanti-Aandanti-Bagglutininsbetweendangerousandnon-dangerousdonors.
Agglutininspecificity Dangerousdonor?a Totaltitrations p-Value
Yes No
Anti-A 88 712 800
0.7468
Anti-B 84 716 800
Totaltitrations 172 1428 1600
Fourtitrationswereperformedforeachsample:anti-AIgM,anti-BIgM,anti-AIgGandanti-BIgG.
a 1:128dilutionswasthecut-offpointforIgMantibodiesand1:256dilutionsforIgGantibodies.
Table2–DistributionofIgMandIgGantibodyclassesbetweendangerousandnon-dangerousdonors.
Antibodyclasses Dangerousdonor?a Totaltitrations p-Value
Yes No
IgM 76 724 800
0.4846
IgG 68 732 800
Totaltitrations 144 1456 1600
Fourtitrationswereperformedforeachsample:anti-AIgM,anti-BIgM,anti-AIgGandanti-BIgG.
a 1:128dilutionswasthecut-offpointforIgMantibodiesand1:256dilutionsforIgGantibodies.
Discussion
Reportsofhemolyticreactionsafterthetransfusionofblood products due to dangerous universal donors are found in theliterature.11Theriskisdirectlyassociatedtothe
hemag-glutinintiterandresidualvolumeofplasmapresent inthe transfusedbloodcomponents.12Itisespeciallyworryingin
platelettransfusion,knowingthattheplatelet concentrates havea considerableamount ofplasma, inparticularthose obtainedbyapheresis.11
InBrazil,hemagglutinintitrationisnotmandatoryinblood banks. According to Ordinance158 05/02/2016, the plasma containedin platelet concentrateswill be ABO compatible withtherecipient’sredbloodcells.Ifthisisnotpossible,it isrecommendedthattheplasmavolumeoftheblood compo-nentandthepresenceofclinicallyrelevantanti-Aandanti-B hemagglutinins(hemolysin) isevaluated whenthe transfu-sion of non-isogroup platelet concentrates is necessary.13
However,accordingtoarecentstudybyLandimetal.,12there
isnocorrelationbetweenhemolysinandtheriskofclinical hemolysisorhemagglutinintitersreinforcingtheimportance ofanalyzing hemagglutinins, which isconsidered the gold standard prophylaxisagainst hemolysisrelated to plasma-incompatibleplatelettransfusions.
Itisworth notingthatit isdifficulttodefine dangerous universal donors with the titers because ofdisagreements regardingtitrationtechniquesandthedelineationofcritical limits. Many studies use a cut-off point of 100 to clas-sify a donor as dangerous using the microplate titration technique.14–18Itshouldbenotedthatstandardizationinthe
reading ofagglutination intensitiesusing this technique is morecomplexcomparedtothetubetechniqueinrespectto thetiterdefinitionoftheAABBTechnicalManual.Thetiter isgivenasthehighestdilutionthatproducesamacroscopic agglutinationofonecross(1+).8
Thisstudyrevealedthat30.5%ofObloodgroupdonorsat thebloodbankinBeloHorizontewereclassifiedasdangerous
universaldonors.Thisresultissimilartothatobtainedinan Italianstudy(27.7%)carriedout in1977,whichinvestigated samplesfrom504donorsandperformedthetitrationsusing thetubetechnique.19
In contrast,aThaistudy founda frequencyof75.7%of dangerousuniversaldonorsduetoanti-AIgMantibodiesand 80.0%duetoanti-BIgMantibodies,whilethefrequenciesof high-riskdonorsduetoanti-AIgGandanti-BIgGantibodies were93.0%and95.3%,respectively.Theresearcherslinkedthe highfrequencyofdangerousdonorstoenvironmentalfactors, differences inthecompositionoftheintestinalmicrobiota, presenceofintestinalparasites,outcomesofvaccinationor exposuretootherantigens.Theyalsonotedthatthenumber offemaledonorshadgrowninrecentyears,whichcanjustify theproportionofhigh-riskdonors,aspregnancyisafactor thatcontributestohigheranti-Aandanti-Bhemagglutinins.20
Notethatthecut-offpointadoptedinthisstudywas64,that islessthanthatinmostotherstudies,whichexplains,inpart, thehighnumberofdangerousdonors.12
Two studiesinvolvingAfricanpopulationsthat aimedto determinethehemolyticactivityofanti-Aandanti-B hemag-glutininsinObloodgroupdonors,byinvestigatinghemolysin reactivity at37◦Crevealed thatinNigeriathe frequencyof
hemolyticactivitywas23.2%.21InZimbabwe,morethan60%
ofplasmafromdonorshadhemolyticactivityandhightiters ofIgGclassantibodies(≥64).Theresearcherscorrelatedthese
findingstothecharacteristicsofthepopulation,suchasthe highincidenceofperinatalhemolyticdiseaseandhistoryof previoustransfusions.22
Another African study aimedto comparethe hemolytic activityofanti-Aandanti-Bintworacialgroups,Blackand WhiteZimbabweans,livingundersimilarconditions.Serum fromBlacksubjectsshowedgreaterhemolyticactivityof anti-A andanti-Bhemagglutinins, whichshows thatthe ethnic background may be an important factor in the hemolytic activityofABOantibodies.23 However,statisticalanalysisof
ethnicityandbeingclassifiedasadangerousuniversaldonor, despitethegreatethniccomplexityoftheBrazilian popula-tion.
Infact, high titers ofhemagglutininsin plasmafrom O bloodgroupwomencanbeexplained,inpart,bygestations offetuses with non-identical ABO blood groups. This may explainthehigherfrequencyofwomenclassifiedas danger-ous universal donors inthis study.There isevidence that perinatal hemolytic disease due to ABO incompatibility is severeinthefirstpregnancy;probablythesecond incompati-blefetuswillalsobeaffectedbythedisease,whichreinforces the theory that high titers of anti-A and anti-B remain in womenforalong time.4,19 Atthe bloodbankinBelo
Hori-zonte,thechanceofawomanbeingclassifiedasadangerous universaldonorwas1.66timeshigherthanmen[oddsratio (OR)=1.66;95%CI=1.08–2.56].
Thehighpercentageofpeoplewhodeclaredthemselves asmulattoreflectsthe greatheterogeneity ofthe Brazilian population. Brazil is considered to have one of the most heterogeneouspopulationsinthe worldresultingfrom the mixingofpeoplefromdifferentcontinents.Inaddition,the vastterritory andthe displacement ofdifferentpopulation groupsindifferentregionsofthecountry hasledtoa con-siderable phylogeographicalheterogeneity.24 Thestatistical
analysisrevealed nosignificantcorrelationbetween ethnic-ityandbeingclassifiedasadangerousuniversaldonor,which probablyreflectsthecomplexethniccategorizationofthe pop-ulation.
Regardingtheagegroup,thedataofthisstudyshowa sig-nificantassociationbetweenyoungdonors(18–28yearsold) andhightitersofhemagglutininscomparedtoolderdonors (49–58yearsold).Itisknownthat,ingeneral,theproductionof anti-Aandanti-Bhemagglutininsstartsbetweenthethirdand sixthmonthsoflife.Thetitersoftheseantibodiesreachpeaks betweentheagesoffiveandtenyears.Afterthat,aprogressive declineinthehemagglutininsisobservedastheindividual ages.4 AtthebloodbankinBeloHorizonte,thechanceofa
youngdonor(18–28yearsold)beingclassifiedasadangerous universaldonorwas3.05 timesgreaterthan 49–58year-old individuals(OR=3.05;95%CI=1.22–7.69).
Thisstudydidnotfindanysignificantassociationbetween the specificity of hemagglutinins and being classified as a dangerousuniversal donor.However,it isknownthat anti-AhemagglutinintiterstendtobehigherintheplasmaofO bloodgroupindividualsthananti-Bhemagglutinintiters.4,25
Moreover,therewasnosignificantassociationbetweenthe antibodyclassandbeingclassifiedasadangerousuniversal donor.Ingeneral, thegoalofautomatedtitration ofanti-A andanti-BhemagglutininsisjusttosearchforIgM antibod-ies becausethere isasignificant association betweenhigh levels ofanti-A and anti-BIgM and hemolysisin vitro and notforIgGantibodies.Thus,thetitrationofanti-Aand anti-BIgMantibodies is recommended totest forincompatible platelettransfusions,especiallyrelatedtofemaleapheresis donors.20
InBrazil,fewstudieshaveinvestigatedthefrequenciesof dangerousuniversaldonorsinbloodbanks.InBotucatu,São Paulo,12.8%ofObloodgroupdonorswereclassifiedas dan-gerous;58.4%duetoanti-AIgMantibodies,14.2%duetoanti-B IgMantibodiesand27.2%duetoboth.16
InSãoJosédosCampos,SãoPaulo,astudythatincluded 6210samplesfromObloodgroupdonorsrevealedafrequency of 13.6% ofdangerous universal donorsdue to anti-A and anti-BIgMantibodies.However,theinfluenceofeach hemag-glutininwasnotdistinguishedandIgGantibodieswerenot evaluated.15
Another study involving4447samples ofOblood group donorsfoundfrequenciesof1.2%ofdonorsclassifiedas dan-gerousuniversaldonorsinItapevaand5.3%inOurinhosboth in São Paulo, without distinguishing the influence ofeach hemagglutininandwithoutassessingIgGantibodies.18
InGuarapuava,Paraná, thefrequencyofdangerous uni-versaldonorswas7.3%(44.4%hadhightitersofanti-AIgM antibodies,35.6%ofAnti-BIgMantibodiesand20%ofboth). IgGantibodieswerenotevaluated.17
Allthesestudieshavecommoncharacteristics:theyused themicroplatetitrationtechniqueafterdilutingthesamples in saline, adopteda titerof over 100to classify donorsas dangerousandonlyevaluatedtheIgMantibodies,whichmay explainthelowfrequencyofdonorsclassifiedasdangerous comparedtothe current study.However,itisimportantto rememberthatitistechnicallydifficulttogradetheintensity ofhemagglutinationusingmicroplates.
Recent Brazilian studies employed the tube titration technique.12,26,27 InSãoPaulo,Franc¸a etal.26 evaluated603
frequentObloodgroupdonorsbyapheresisorwhoseblood componentswould betransfusedinnewborns;only13%of donorspresentedhightitersofhemagglutinins(cut-offpoint >64). The IgG antibodies were not evaluated, which may explainthelowfrequencyofdangerousuniversaldonors. Var-gasetal.,27inPortoAlegre,RioGrandedoSul,evaluated610O
bloodgroupdonorswhoweredonatingplateletsbyapheresis andfoundafrequencyof50.7%ofdonorswithhightitersof anti-Aantibodiesand41.5%ofanti-Bantibodies.The method-ologyusedinthisstudywasthetubetechniquediluted1:100 insaline.Theresultsweresimilartothecurrentstudy,butthe IgGantibodieswerenotevaluated.
Somemethodologicaldifferencesthatmayinfluencethe resultsobtainedinstudiesconductedinBrazilcanbe men-tioned.Thesedifferencesincludeperformingserialdilutions ofsamplesorjustdiluting1:100insaline,thetimeof incu-bation beforereading, aspectsrelated to the calibrationof equipment(centrifugesandpipettes)andthesubjectivityof readings.OnrememberingthesizeofBrazil,itisworthnoting thatdifferencesinthecharacteristicsofthepopulationmight justifythedifferencesinfrequenciesofdangerousuniversal donorsindifferentstudies.
Conclusion
steptowardmakingtransfusiontherapysaferforpatientswho benefitfrombloodcomponentsfromObloodgroupdonors.
Funding
Fundac¸ãodeAmparoàPesquisadeMinasGerais(FAPEMIG), Conselho Nacional de Desenvolvimento Científico e Tec-nológico(CNPQ)andFundac¸ãoHemominas.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
r
e
f
e
r
e
n
c
e
s
1. FiglM,PelinkaLE.KarlLandsteiner,thediscovererofblood groups.Resuscitation.2004;63(3):251–4.
2. OttenbergR.Studiesinisoagglutination–transfusionandthe questionofintravascularagglutination.JEM.1911:425–38. Availablefrom:http://jem.rupress.org/content/13/4/425.long
[cited15.09.13].
3. HarmeningDM,FirestoneD.SistemaSanguíneoABO.In: HarmeningDM,editor.TécnicasModernasemBancode SangueeTransfusão.RiodeJaneiro:EditoraRevinter;2006.p. 90–125.
4. KleinHG,AnsteeDJ,editors.Mollison’sbloodtransfusionin clinicalmedicine.11thed.2005,891pp.
5. LevineP,MabeeJ.Adangerousuniversaldonordetectedby thedirectmatchingofbloods.JImmunol.1923;8:425–31.
6. BarnettV.SampleSurvey:principlesandmethods.London: Arnold;2009,258pp.
7. JosephsonCD,CastillejoMI,GrimaK,HillyerCD.
ABO-mismatchedplatelettransfusions:strategiestomitigate patientexposuretonaturallyoccurringhemolyticantibodies. TransfusApherSci.2010;42(1):83–8.
8. RobackJD,GrossmanBJ,HarrisT,HillyerCD,editors. Technicalmanual.17thed.Bethesda,MD:American AssociationofBloodBanks;2011.
9. CoolingL.ABOandplatelettransfusiontherapy. Immunohematology.2007;23(1):20–33.
10.JosephsonCD,MullisNC,DemarkCV,HillyerCD.Significant numbersofapheresis-derivedgroupOplateletunitshave high-titeranti-A/A,B:implicationsfortransfusionpolicy. Transfusion.2004;44(6):805–8.
11.LozanoM,CIDJ.Theclinicalimplicationsofplatelets transfusionsassociatedwithABOorRh(D)incompatibility. TransfusMedRev.2003;17(1):57–68.
12.LandimCS,GomesFC,ZezaBM,Mendrone-JúniorA,Dinardo CL.Prophylacticstrategiesforacutehemolysissecondaryto plasma-incompatibleplatelettransfusions:correlation
betweenqualitativehemolysintestandisohemagglutinin titration.RevBrasHematolHemoter.2015;37(4):217–22.
13.DiarioOficialdaUnião(DOU)PortariaN◦158,de4defevereiro
de2016.Redefineoregulamentotécnicodeprocedimentos hemoterápicos.
14.NovarettiMC.Hemolisinasanti-Aeanti-Bnaprática transfusional.VerBrasHematolHemoter.2008;30(6):433–6.
15.RosaES,MeloDB,MeloCM,FelipeLF.Frequênciadedoadores Ocomhemolisinasemaltostítulos:experiênciadoServic¸o deHemoterapiadeSãoJosédosCampos.RevBrasHematol Hemoter.2004;26(3):224.
16.GamberoS,SeccoVN,FerreiraRR,DeffuneE,MachadoPE. Frequênciadehemolisinasanti-Aeanti-Bemdoadoresde sanguedoHemocentrodeBotucatu.RevBrasHematol Hemoter.2004;26(1):28–34.
17.CosechenVS,PittnerE,KhalilNM,HorstS,MonteiroMC. Frequênciadeaglutininasanti-Aeanti-Bnosdoadoresde sanguedogrupo‘O’doHemonúcleodeGuarapuava(PR). RevistaSalus-Guarapuava(PR).2009;3(1):39–48.
18.FernandesVC,BorgattoAF,FilhoSB,ToledoMI,LopesLC. Frequênciadehemolisinasanti-Aeanti-Bemdoadoresde sanguedeItapevaeOurinhos.RevBrasHematolHemoter. 2008;30(6):453–6.
19.DeBartoloM,GiordanoF,ViolanteA,BonomiP.Laboratory testsappliedtotransfusionproblems.Identificationof dangerousuniversaldonorsandtheirfrequency.AnnSclavo. 1977;19(5):1092–102.
20.KhampanonK,ChanprakopT,SriwanitchrakP,SetthakarnM, OotaS,NathalangO.ThecharacteristicsofABOantibodiesin groupOThaiblooddonors.JClinLabAnal.2012;26(4):223–6.
21.OlawumiHO,OlatunjiPO.Prevalenceandtitreofalphaand betahaemolysinsinbloodgroup‘O’donorsinIlorin.AfrJ MedMedSci.2001;30(4):319–21.
22.AdewuyiJO,GwanzuraC,MvereD.Characteristicsofanti-A andanti-BinblackZimbabweans.VoxSang.1994;67(3): 307–9.
23.AdewuyiJO,GwanzuraC.Racialdifferencebetweenwhite andblackZimbabweansinthehaemolyticactivityofA,B,O antibodies.AfrJMedMedSci.2001;30(1–2):71–4.
24.ParraFC,AmadoRC,LambertucciJR,RochaJ,AntunesCM, PenaSD.ColorandgenomicancestryinBrazilians.Genetics. 2003;100(1):177–82.
25.AubertEF,DoddBE,BoormanKE,LoutitLF.Theuniversal donorwithhightitreiso-agglutinins–theeffectofanti-A iso-agglutininsonrecipientsofgroupA.BrMedJ. 1942;1(4247):659–64.
26.deFranc¸aND,PoliMC,RamosPG,BorsoiCS,ColellaR.Titers ofABOantibodiesingroupOblooddonors.RevBrasHematol Hemoter.2011;33(4):259–62.