RevBrasAnestesiol.2015;65(4):298---301
REVISTA
BRASILEIRA
DE
ANESTESIOLOGIA
OfficialPublicationoftheBrazilianSocietyofAnesthesiologywww.sba.com.br
CLINICAL
INFORMATION
Anesthetic
management
for
surgery
of
esophagus
atresia
in
a
newborn
with
Goldenhar’s
syndrome
Rosana
Guerrero-Domínguez
a,∗,
Daniel
López-Herrera-Rodríguez
a,
Inmaculada
Benítez-Linero
a,
Antonio
Ontanilla
baServiceofAnesthesiologyandReanimation,HospitalesUniversitariosVirgendelRocío,Sevilla,Spain
bServiceofAnesthesiologyandReanimation,HospitalInfantil,HospitalesUniversitariosVirgendelRocío,Sevilla,Spain
Received3July2013;accepted25July2013 Availableonline28April2015
KEYWORDS
Goldenhar’s syndrome;
Tracheoesophageal fistula;
Esophagealatresia; Difficultairway; Fibrobronchoscope
Abstract
Backgroundandobjectives: Goldenhar’ssyndromeisapolymalformativeconditionconsisting ofacraniofacialdysostosisthatdeterminesdifficultairwayinupto40%ofcases.Wedescribed acaseofanewbornwithGoldenhar’ssyndromewithesophagealatresiaandtracheoesophageal fistulawhounderwentrepairsurgery.
Casereport: Wereportthecaseofa24-h-oldnewborn withGoldenhar’ssyndrome. Hehad
esophageal atresiawithdistal tracheoesophagealfistula.Itwas decidedthatanemergency
surgerywouldbeperformedforrepairingit.Itwascarriedoutundersedation,intubationwith fibrobronchoscopedistaltothefistula,tolimittheairflowintotheesophagus,andpossible abdominal distension.Following complete repair ofthe esophagealatresia andfistula liga-tion,thepatientwastransferredtotheintensivecareunitandintubatedundersedationand analgesia.
Conclusions:The finding of a patient with Goldenhar’s syndrome and esophageal atresia assumesanexceptional situationandachallengefor anesthesiologists,sincetheanesthetic
managementdependsonthepatientcomorbidity,thetypeoftracheoesophagealfistula,the
usualhospitalpracticeandtheskillsoftheanesthesiologistincharge,withthemain
peculiar-itybeingmaintenanceofadequatepulmonaryventilationinthepresenceofacommunication
betweentheairwayandtheesophagus.Intubationwithfibrobronchoscopedistaltothefistula dealswiththemanagementofaprobablydifficultairwayandlimitsthepassageofairtothe esophagusthroughthefistula.
©2013SociedadeBrasileiradeAnestesiologia.PublishedbyElsevier EditoraLtda.Allrights reserved.
∗Correspondingauthor.
E-mail:[email protected](R.Guerrero-Domínguez).
SurgeryforesophagealatresiainnewbornwithGoldenhar’ssyndrome 299
PALAVRAS-CHAVE
Síndromede Goldenhar; Fístula
traqueoesofágica; Atresiadeesôfago; Viarespiratória difícil;
Fibrobroncoscópio
Manejoanestésicoparacirurgiadeatresiadeesôfagoemumrecém-nascidocom síndromedeGoldenhar
Resumo
Justificativaeobjetivos: AsíndromedeGoldenharéumquadrodepolimalformac¸ãoque con-sisteemumadisostosecraniofacialquedeterminaumaviarespiratóriadifícilematé40%dos
casos.Nósdescrevemosumcasodeumrecém-nascidocomsíndromedeGoldenharcomatresia
deesôfagoefístulatraqueoesofágicaparaaqualfoirealizadacirurgiadereparo.
Relatodecaso: Apresentamosocasodeumrecém-nascidode24hdevidacomsíndromede Goldenhar.Eleapresentavaatresiadeesôfago,comfístulatraqueoesofágicadistal. Decidiu-seporumacirurgiadeemergênciaparareparo.Elafoirealizadasobsedac¸ão,intubac¸ãocom fibrobroncoscópiodistalàfístula,paralimitarpassagemdoarparaoesôfagoepossíveldistensão abdominal.Apósoreparocompletodaatresiadeesôfagoeligaduradafístula,opacientefoi transferidoparaaunidadedeterapiaintensivaeintubadocomsedoanalgesia.
Conclusões: OachadodeumpacientecomsíndromedeGoldenhareatresiadeesôfagosupõe
uma situac¸ão excepcionaleum desafiopara os anestesiologistas,pois omanejoanestésico
dependedacomorbidadedopaciente,dotipodefístulatraqueoesofágica,dapráticahospitalar habitualedashabilidadesdoanestesiologistaresponsável,sendoqueapeculiaridadeprincipal
émanter umaventilac¸ãopulmonaradequadanapresenc¸ade umacomunicac¸ãoentreavia
respiratóriaeoesôfago.Aintubac¸ãocomfibrobroncoscópiodistalàfístularesolveomanejo daviarespiratóriaprovavelmentedifícilelimitaapassagemdearparaoesôfagoatravésda fístula.
©2013SociedadeBrasileira deAnestesiologia.PublicadoporElsevierEditoraLtda.Todosos direitosreservados.
Introduction
Goldenhar’ssyndrome(GS)oroculo-auriculo-vertebral dys-plasia was first described by von Arlt in 1845.1 This is a
polymalformative condition resulting from defects of the firstandsecond branchialarchs1 consistingof craniofacial
dysostosis,whereweobserveabnormalitiesoftheeyesand cervical vertebrae, malformations of the ears and unilat-eralmicrothia,facialasymmetry,micrognathia,2epibulbar
dermoidcysts1andotherchangesoftheoralcavity,suchas
cleftpalateandlingualchange.3,4Althoughtheincidenceof
GSisestimatedat1in5000livenewborns,2,4theassociation
ofesophagealatresia(EA)andthisconditiononlyoccursin 5%ofthesepatients,1andisanexceptionalcombination.
Clinical
case
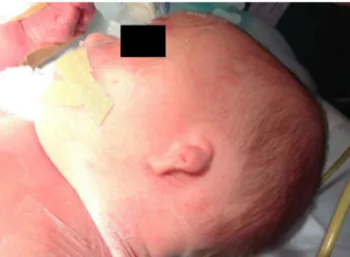
Wepresentacaseofa24-h-oldnewbornof3.2kgofweight withleftunilateralmicrothia(Fig.1),bilateralureterocele and esophageal atresia with distal tracheoesophageal fis-tula(TEF).Anemergencysurgerywaschosentorepairthe EA andassociatedfistula. On examinationof theairways, mildmicrognathiaanddifficultopeningofthemouthwere found.As supplementarypreoperativetests,achestX-ray withnasogastrictubewasperformed,whichconfirmedthe diagnosis(Fig.2),alongwithbloodcount,biochemistryand coagulationstudy,transthoracicechocardiographyand elec-trocardiography,whichshowednochanges.
In the operating room monitoring was performed with non-invasive blood pressure, pulse oximetry (SpO2),
and electrocardiogram. Under sedation with 2% sevoflu-rane, 0.1mg IV atropine through a venous access with
epicutaneouscatheterwasgiventoreduce oropharyngeal secretions, as well as 10g fentanyl. With the patient underspontaneous ventilation the fibrobronchoscope was introducedbymouthuptotheopeningof theglottis,and a rigid tube of 3.5mm in diameter was inserted, being positioned distal to the TEF and near the main carina. The proper placement of the endotracheal tube (ETT) wasconfirmedbycapnographyandpulmonaryauscultation, startingvolume-controlledventilationwithatidalvolumeof 8mlkg−1andrespiratoryratebetween17and20.To main-taintheanesthetic, the concentrationof sevoflurane was increasedto3%and1mgcisatracuriumindosesof6---9gof fentanylweregiven,accordingtotheneedforpainkillers.
300 R.Guerrero-Domínguezetal.
Figure2 Radiologicalimage showing aturn of nasogastric tubeduetoimpossibilityofadvancingitinesophageallevel.
During surgery the patient remained hemodynamically stable with a heart rate of 140---150 beats per minute andsystolicbloodpressurebetween70and75mmHg.The respiratorysystemkeptSpO2 at90---95%which surprisingly
reached values close to 100% after complete repair of esophagealatresia andligationof thefistula.The surgery lasted170min withadministrationof40mlof crystalloids withnoneedfortransfusionsofbloodproducts.Upon com-pletion of the surgical procedure, he was transferred to theintensive care unitwithsedoanalgesia, intubatedand mechanicallyventilated,withnocomplications.
Discussion
Craniofacial changes in GS can condition a difficult air-way(DAW) in up to40% of thecases,5 mainly due tothe
combination of micrognathia, limitation of cervical joint movement, and tracheal shift.5,6 This is a challenge for
anesthesiologists and may require the use of alternative methodsfor thedirect laryngoscopytoensure proper air-waypatency, such asintubation withfibrobronchoscope,6
theuseoflaryngealmaskLMA4andalsotheperformanceof
tracheostomywith retrograde intubation.4,5 A mandibular
andcraniocervicalradiologicalevaluationbeforescheduled surgicalproceduresis recommended.7 Othermedical
con-ditions associated with this syndrome, such as cardiac, tracheoesophageal, genitourinary anomalies, and mental retardment1,2shouldberuledout.
TheEA,withorwithoutTEF,isthemostcommon congen-italesophagealanomaly,withanincidencerangingfrom1in 2500---4500livenewborns.2TheclassificationofEAis
deter-minedbythelocationofatresiaandthepresenceorabsence ofassociatedTEF.Fivedifferenttypes weredescribed, so thatEAwithdistal fistulaassumes 85%of thecases.8 The
diagnosisofEAisconfirmedbytheinabilitytomakea naso-gastrictubemovetothestomach,abundantoralsecretions andcoughingorepisodesofcyanosisafterfoodingestion.8A
chestX-raywithanasogastricororogastrictubecanprovide confirmationofthediagnosis.8AlthoughThomasGibsonhad
describedEAassociatedwithTEFin1697,itwasonlyin1941
thatCameronHaightperformedthefirstsurgicalcorrection ofthisproblem.9SurgerytorepairEAandTEFhasimportant
anestheticimplications10andisachallengefor
anesthesiol-ogists.Often,newborns mayhaverespiratorydiseasesand associatedcardiacmalformationsthat,alongwithaweight oflessthan2kg,areriskfactorsforpostoperativemortality andshouldbeassessedpriortosurgery.10,11
Themainfeatureoftheanestheticmanagementinthis surgeryis themaintenance ofadequate ventilationin the presenceofacommunicationbetweentheairwayandthe esophagus, and desaturation episodes may occur during inductionandduringanestheticmaintenance.Ontheother hand,theperformanceofathoracotomymaydeterminethe presentationofhemodynamicandrespiratorychanges,and difficultmaintenanceofanappropriatelevelofanalgesia.10
Theanestheticmanagementdependsonpatient comorbidi-ties,thetypeofEAwithorwithoutTEF,theusualhospital practice,andtheskillsoftheanesthesiologistincharge.
NewbornswithTEF areatincreasedrisk ofgastric dis-tension with potential risk of pneumoperitoneum11 which
canincreasewiththeintroductionofmechanicalventilation withpositivepressure.DuringrepairofTEFthereareseveral alternativesforthemaintenanceofmechanicalventilation, suchasleftbronchialselectiveintubation,11 assuming the
riskofatelectasis,andintubationwith fibrobronchoscope-guidedplacementofETTdistaltothefistula,whichwasthe techniqueusedinthiscase.11 BothformsofETTplacement
requireclosemonitoringbytheanesthesiologistinchargeto detectabadpositioningofthetubeduringtheprocedure. Anothertechniquethatcouldbeusedistheocclusionofthe fistulausingaFogartycatheteruntilitscompleteligation.12
Itisrecommendedthatspontaneousventilationis main-tainedthroughinhalationinductionwithoutneuromuscular blockade nor positive pressure ventilation until the cor-rectplacementoftheETTisachieveddistaltothefistula8
toavoid gastric hyperinflation. Other authors recommend maintaining spontaneous ventilation tothe complete clo-sureofthefistulatominimizegastricdistensionassociated withpositivepressureventilation,withsome anesthesiolo-gistsevenrecommendingtheperformanceofagastrostomy beforeanestheticinductiontodecompressthestomachand improvemechanicalventilation.11,12
Inthecase ofGS, thefindingofaDAWassociatedwith EA with TEF could seriously impair oxygenation in these patients duringanesthetic induction, significantly increas-ing the risk of respiratory complications that are already highduetothesurgicalprocedureitself.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
References
1.AyusoVelascoR,TorresAguirreA,EnríquezZarabozoE,etal. Atresiade esófagoenelsíndromedeGoldenhar.Cir Pediatr. 2010;23:65.
SurgeryforesophagealatresiainnewbornwithGoldenhar’ssyndrome 301
3.OrtegaU,BejarJ,MartínezE.Managementofanaesthesiaand theairwayinachildwithGoldenharsyndrome.RevEsp Aneste-siolReanim.2012;59:110---2.
4.Sukhupragarn W, Rosenblatt WH. Airway management in a patientwithGoldenharsyndrome:acasereport.JClinAnesth. 2008;20:214---7.
5.AhmedZ,AlalamiA,HaupertM,etal.Airwaymanagementfor rigidbronchoscopyviaafreshlyperformedtracheostomyina childwithGoldenharsyndrome.JClinAnesth.2012;24:234---7. 6.OzlüO,Sims¸ekS,Alac¸akirH,etal.Goldenharsyndromeand intubationwiththefiberopticbroncoscope.PaediatrAnaesth. 2008;18:793---4.
7.AltintasF,CakmakkayaOS.Generalanesthesiaforachildwith Goldenharsyndrome.PaediatrAnaesth.2005;15:529---30.
8.PassiY,SampathiV,PierreJ,etal.Esophagealatresiawith dou-bletracheoesophagealfistula.Anesthesiology.2013;118:1207. 9.Pinheiro PF, Simões e Silva AC, Pereira RM. Current
knowl-edgeonesophagealatresia.WorldJGastroenterol. 2012;28: 3662---72.
10.Knottenbelt G, CostiD,Stephens P,et al.Anauditof anes-theticmanagement and complicationsoftracheo-esophageal fistula and esophageal atresia repair. Paediatr Anaesth. 2012;22:268---74.
11.BroemlingN,CampbellF.Anestheticmanagementofcongenital tracheoesophagealfistula.PaediatrAnaesth.2011;21:1092---9. 12.Goswami D, Kachru N, Pant N. Difficult ventilation in a