rev bras reumatol.2015;55(2):174–176
w w w . r e u m a t o l o g i a . c o m . b r
REVISTA
BRASILEIRA
DE
REUMATOLOGIA
Case
report
Relapsing
polychondritis
with
severe
hearing
loss
Francisco
Vileimar
Andrade
de
Azevedo
∗,
Juliana
de
Deus
e
Albuquerque,
Deborah
Pereira
Gonc¸alves
HospitalGeralDr.WaldemarAlcântara,Fortaleza,CE,Brazil
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received3October2013 Accepted20March2014 Availableonline5January2015
Keywords:
Policondritis Auditiveloss Vasculitis
a
b
s
t
r
a
c
t
Relapsingpolychondritisisanuncommon,immune-mediatedconditioncharacterizedby episodesofinflammationofcartilaginousstructures,especiallytheears,nose,jointsand respiratorytract.RPalsoaffectsproteoglycan-richstructuressuchastheeyes,heart,blood vesselsandinnerear.Aroundonethirdofcasesareassociatedwithotherdiseasessuchas vasculitides,connectivetissuediseasesormyelodysplasticsyndrome.Disordersoftheinner earoccurin40–50%ofpatients.Profoundhearinglossisrare.Theaimofthisstudywasto describethecaseofapatientwithrelapsingpolychondritisassociatedwithseverebilateral hearinglossandclinicalmanifestationsofsystemicvasculitis.Thisstudyreinforcesthe importanceofanearlydiagnosisandimmediatetreatmentincaseofseveremanifestations ofthedisease.
©2014ElsevierEditoraLtda.Allrightsreserved.
Policondrite
recidivante
com
perda
auditiva
severa
Palavras-chave:
Policondrite Perdaauditiva Vasculite
r
e
s
u
m
o
Policondriterecidivanteéumacondic¸ãorara,imunomediada,caracterizadaporepisódios deinflamac¸ãodeestruturascartilaginosas,principalmenteorelhas,nariz,articulac¸õese sistemarespiratório.Acometetambém estruturas ricasem proteoglicanoscomo olhos, corac¸ão, vasos sanguíneos e ouvido interno. Em torno de 1/3 dos casos apresentam associac¸ãocomoutrasdoenc¸ascomovasculitessistêmicas,doenc¸asdotecidoconectivoou síndromemielodisplásica.Desordensdoouvidointernoocorremem40%-50%dospacientes. Perdaauditivaprofundaérara.Oobjetivodoestudofoidescreverocasodeumapaciente comdiagnósticodepolicondriterecidivanteassociadoàperdaauditivaseverabilaterale manifestac¸õesclínicasdevasculitesistêmica.Estetrabalhoreforc¸aaimportânciado diag-nósticoprecoceedotratamentoimediatoemcasodemanifestac¸õesseverasdadoenc¸a.
©2014ElsevierEditoraLtda.Todososdireitosreservados.
∗ Correspondingauthor.
E-mail:[email protected](F.V.A.deAzevedo). http://dx.doi.org/10.1016/j.rbre.2014.03.029
rev bras reumatol.2015;55(2):174–176
175
Introduction
Relapsing polychondritis (RP) is a rare, immune-mediated conditioncharacterizedbyepisodesofinflammationof car-tilaginous structures, especially the ears, nose, joints and respiratorysystem.Italsoaffectsproteoglycan-richstructures suchastheeyes,heart,bloodvesselsandinnerear.The dis-easewasfirstdescribedin1923byJaksch-Wartenhorst,who namedthediseasepolicondropathy.Pearsonetal.introduced thetermpolychondritisin1960.1Theconditionaffectsmen
and womenequally and can beseen inall races. Itspeak incidenceisbetween40and60years.2
TheetiologyofRPisunknown.Thegeneticpredisposition issuggestedbytheassociationwithleukocyteantigen HLA-DR4.3Thereisevidencefortheemergenceofautoimmunity,
bothhumoralandcellular, againstcartilagematrix compo-nentssuchascollagentypesII,IX,XIandmatriline-1.2
WereportthecaseofRPassociatedwithseverehearing lossandvasculiticskinlesions.
Case
report
DMD, 31 years old, female, with an everyday fever for twomonths, associated withchills, asthenia,polyarthritis, progressivebilateral hearing loss, tinnitus and episodes of dizziness.Amonthago,hercaseevolvedwiththeappearance ofskinlesionsonthehandsandlowerlimbs,bilateraledema intheeyelidsand ears,andacontinuouspaininthedistal regionof2ndrightfinger.
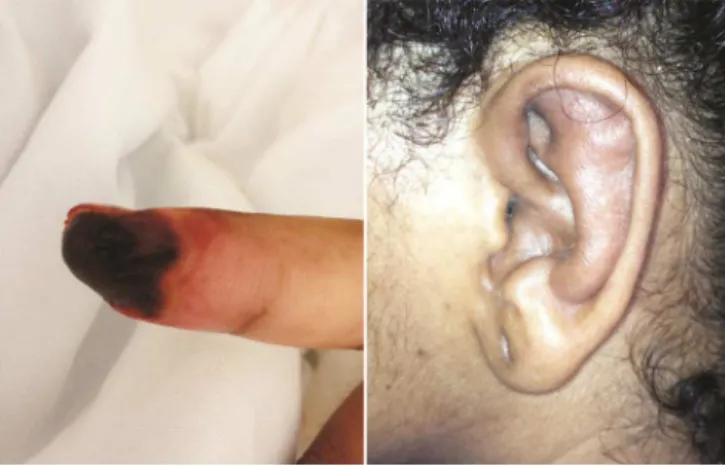
Aphysicalexaminationrevealedarthritisinwrists,elbows, ankles and proximal interphalangeal joints bilaterally. Her skin lesions were characterized by papules, pustules and purplish plaques on the hands, feet and anterior legs. In heroropharynx,aphthousulcerswereobserved.Itwasalso noticedalobe-sparingswellingandpainonpalpationinher pinnae,andbilateralconjunctivaledemaanderythema.The distal region of 2nd right finger exhibited a fixed painful cyanosis,associatedwithlowertemperatures(Fig.1).
Complementary tests showed normocytic and
nor-mochromic anemia (hemoglobin 7.9g/dL), leukocytosis of 16,000mm3 without shift, and elevation of inflammatory markers: C-reactive protein (CRP 196mg/L), erythrocyte
Fig.1–Left,vasculiticinjuryin2ndrightchirodactyl.Right, edemainthepinna,sparingtheearlobe.
Fig.2–Hyalinecartilage(pinna)containingnumerous inflammatorycellswithmatrixdegeneration.
(Hematoxylin–eosin–100×).Inset:evidenceofinfiltrate
withnumerousneutrophils,inassociationwith lymphocytesandhistiocytes(400×).
sedimentation rate (ESR, 45mm within 1h). Serology for hepatitisBand CandHIVwerenegative,andthepresence ofautoantibodies(antinuclearantibody,antineutrophil cyto-plasmicantibody,rheumatoidfactor)andcryoglobulinswere negative,aswellasforAFBinlymph.DirectCoombs,dosage ofcomplements,urinalysisandliverandrenalfunctionswere within normal standards. High digestive endoscopy, chest radiography, abdominal ultrasound, and Doppler forlimbs werenormal.Theechocardiogramshowednochanges.Blood and urine cultures showed no growth of microorganisms. Biopsiesofskinlesionswereperformedinthe2ndrightfinger andpinna.
The diagnosis ofrelapsing polychondritis was proposed based on the clinical manifestationsfound and on results of complementary tests. In the light of these findings, a treatment with prednisone 1mg/kg/day was initiated. The condition progressed to resolution of fever, conjunctival lesionsandjointconditions,butwithnoimprovementofthe deafnessandofischemiainthe2ndchirodactylafteraweek oftreatment.Atthatmoment,itwasdecidedtostartpulse therapywithmethylprednisolone1g/dayforthreedays.
The histopathology of the pinna showed the cartilage withlymphocyticandneutrophilicinfiltrateassociatedwith degenerationofhyalinematrix(Fig.2).Thehistopathologyof cutaneous lesionsoftheright hand revealednecrosiswith extensiveinfiltrationofneutrophilsandlymphocytes.
176
rev bras reumatol.2015;55(2):174–176Discussion
Patientswithrelapsingpolychondritisexhibitabroad spec-trumofclinicalsignsandsymptomsthatoftenincreasethe diagnosticchallenge.Thediagnostic criteriahavebeen pro-posedbyMacAdam,andrequirethreeormoreofthefollowing clinicalfeatures: bilateralauricular chondritis,seronegative non-erosive polyarthritis, nasal chondritis, ocular inflam-mation, respiratory tract chondritis and vestibulocochlear dysfunction.4Arecentmodificationofthesecriteriasuggests
thatthediagnosis canbemadebythe presenceofatleast oneoftheMacAdamcriteria,inassociationwithhistological confirmation ofcartilage damage or chondritisin two dis-tinctanatomicalregions,withresponsetocorticosteroidsor dapsone.5
Thepatientdescribedhadbilateralchondritisofthepinna, bilateralconjunctivitis,seronegativenon-erosive polyarthri-tis,sensorineuralhearinglossandcompatible histopatholog-icalfindings,incompliancewithcriteriaforthediagnosisof RP.Apinnabiopsywasperformed,butthehistopathologyis notalwaysnecessarytoconfirmthediagnosis.
Earlydiagnosisisadifficulttask.TrenthamandLereported thatthe average timeto its establishmentisof2.9years.6
Themostfrequentclinicalmanifestationisanunilateralor bilateralinflammationoftheearcartilage,withanincidence rangingfrom43to83%.Arthritisisthesecondmostcommon manifestation.Aroundonethirdofcasesoccurinassociation withother diseases suchas systemicvasculitides, connec-tivetissuediseasesormyelodysplasticsyndrome.2Inthecase
reported, besidesauricular chondritis and polyarthritisthe patienthadseveresensorineuralhearinglossand vasculitis-compatiblecutaneousmanifestations.
Disordersoftheinnerearoccurin40–50%ofpatients. Pro-foundhearinglossisrare.3,7Itwasreportedanassociationof
cutaneousvasculitisandseverehearingloss,butthe patho-genesisofthissensorineural injuryisstilluncertain.There isapossibilityofanobliterativevasculitisintheinner audi-toryartery,causing otologicalinjury.8,9 Anotherhypothesis,
raisedbyIssingetal.,wouldbethepresenceofantilabyrinth antibodies in the serum of patients with audiovestibular dysfunction.10
Mucocutaneousmanifestationsoccurinmorethan50%of cases;aphthousulcersarethemostcommonchange.2A
his-tologicalevaluationofskinlesionshasshownleukocytoclastic vasculitis,neutrophilicinfiltratesandthrombosisofskin ves-selsmoreoften.11
Vasculitisishistologicallyobservedin14–25%ofcasesand canbeindolentorfulminant; additionally,itandcanoccur simultaneouslyorindependentlyofothermanifestations.12
Drug treatment in patients with chondritis or arthritis shouldbestartedwithnonsteroidalanti-inflammatorydrugs, dapsoneorcorticosteroids.Inthosepatientswithsevere man-ifestations,systemicvasculitisorsensorineuralhearingloss, prednisone1mg/kg/day orpulse therapywith methylpred-nisolone is the treatment ofchoice. In casesof resistance tosteroids,otherimmunosuppressiveagents,including aza-thioprine,methotrexateandcyclophosphamide,arereported asbeinguseful.Isolatedcasereportswerepublished show-ing potentiallybeneficial resultswithantagonists oftumor
necrosisfactor.2Inthecasereported,prednisone1mg/kg/day
wasstartedinapatientwithaclinicalpicturecompatiblewith cutaneousvasculitisandsevereinjuryinherinnerear.Asthe conditionhasnotevolvedwiththeexpectedimprovementof itsmostseveremanifestations,wedecidedinfavorofpulse therapywithmethylprednisoloneandcyclophosphamide.
Itisestimatedthatthefive-yearsurvivalis74%.Patients youngerthan51yearsoldandwithsystemicvasculitishavea worseprognosis.13
Relapsing polychondritis is a multisystem disease with variable presentation, which,inits spectrumof manifesta-tions,canleadtoseriousand irreversibledamagetotarget organs.Itislikely,thatinthecasereported,thepermanence ofa severehearing sequel,evenwiththe institutionofan aggressive therapy, is explained by the long time elapsed fromtheonsetofclinicalmanifestationstothediagnosisand institutionoftherapy.Anearlydiagnosis,combinedwithan aggressivetherapyincasesofseveremanifestations,can pro-ducebeneficialeffectsinthepreventionofserioussequelae.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
r
e
f
e
r
e
n
c
e
s
1.PearsonMC,KlineMH,NewcomerDV.Relapsing polychondritis.NEnglJMed.1960;263:51–8.
2.GergelyPJr,PoorG.Relapsingpolychondritis.BestPractRes ClinRheumatol.2004;18:723–38.
3.ZeunerM,StraubRH,RauhG,AlbertED,SchölmerichJ,Lang B.Relapsingpolychondritis:clinicalandimmunogenetic analysisof62patients.JRheumatol.1997;24:96–101. 4.McAdamLP,O’HanlanAM,BluestoneR,RearsonCM.
Relapsingpolychondritis:prospectivestudyof23patients andareviewoftheliterature.Medicine(Baltimore). 1976;55:193–215.
5.DamianiJM,LevineHL.Relapsingpolychondritis–reportof tencases.Laryngoscope.1979;89:929–46.
6.TrenthamDE,LeCH.Relapsingpolychondritis.AnnIntern Med.1998;129:114–22.
7.CodyDTR,SonesDA.Relapsingpolychondritis: audiovestibularmanifestations.Laryngoscope. 1971;81:208–22.
8.SchuknechtH.Earpathologyinautoimmunedisease.Adv OtoRhinoLaryngol.1991;46:50–70.
9.MichetC.Vasculitisandrelapsingpolychondritis.RheumDis ClinNAm.1990;16:441–4.
10.IssingWJ,SeloverD,SchulzP.Anti-labyrinthineantibodiesin apatientwithrelapsingpolychondritis.EurArch
Otorhinolaryngol.1990;256:163–6.
11.FrancesC,elRassiR,LaporteJL,RybojadM,PapoT,PietteJC. Dermatologicmanifestationsofrelapsingpolychondritis.A studyof200casesatasinglecenter.Medicine(Baltimore). 2001;80:173–9.
12.BarzegarC,VrtovsnikF,DevarsJF,MignonF,PradalierA. VasculitiswithmesangialIgAdepositscomplicatingrelapsing polychondritis.ClinExpRheumatol.2002;20:89–91.