RevBrasAnestesiol.2017;67(2):210---213
REVISTA
BRASILEIRA
DE
ANESTESIOLOGIA
PublicaçãoOficialdaSociedadeBrasileiradeAnestesiologiawww.sba.com.br
CLINICAL
INFORMATION
Anesthetic
management
of
an
infant
with
giant
abdominal
neuroblastoma
Manuel
Ángel
Gómez-Ríos
∗,
Federico
Curt
Nu˜
no,
Purísima
Barreto-Calvo
ComplejoHospitalarioUniversitariodeACoru˜na,DepartamentodeAnestesiologíayMedicinaPerioperatoria,ACoru˜na,Spain
Received6July2014;accepted21July2014 Availableonline8November2014
KEYWORDS
Neuroblastoma; Pediatricanesthesia; Infant;
Hypertension
Abstract Neuroblastomaisthemostcommon,non-centralnervoussystemtumorofchildhood. Ithas thepotential to synthesizecatecholamines. However, the presences ofhypertension areuncommon.Wereporttheperioperativemanagementofa15-month-oldinfantwithgiant abdominalneuroblastomawho presentedseverehypertension.Thepathophysiological alter-ationsofneuroblastomaarereviewedandperioperativemanagementpresented.
©2014SociedadeBrasileiradeAnestesiologia.PublishedbyElsevierEditoraLtda.Thisisan openaccessarticleundertheCCBY-NC-NDlicense( http://creativecommons.org/licenses/by-nc-nd/4.0/).
PALAVRAS-CHAVE
Neuroblastoma; Anestesiapediátrica; Crianc¸a;
Hipertensão
Manejoanestésicodecrianc¸acomneuroblastomaabdominalgigante
Resumo Neuroblastoma é otumor mais comum do sistema nervoso não-centralna infân-cia. Esse tumor tem o potencial para sintetizar catecolaminas; entretanto, a presenc¸a de hipertensão érara. Relatamos o manejoperioperatório deuma crianc¸a de cinco mesesde idadecomneuroblastomaabdominalgigantequeapresentouhipertensãograve.Asalterac¸ões fisiopatológicasdoneuroblastomaforamrevistaseomanejoperioperatórioapresentado. ©2014SociedadeBrasileiradeAnestesiologia.PublicadoporElsevierEditoraLtda.Este ´eum artigoOpen Accesssobumalicenc¸aCCBY-NC-ND( http://creativecommons.org/licenses/by-nc-nd/4.0/).
Introduction
Neuroblastomaisthemostcommonextracranialsolidtumor
in childhood.1 It affects yearly 6---10 million of children,
∗Correspondingauthor.
E-mail:[email protected](M.Á.Gómez-Ríos).
accounting7---8% ofpediatrictumors.Clinicalpresentation
is highly variable depending on location. It may include
nonspecific signs and symptoms such as abdominal pain,
vomiting,weightloss,anorexia,fatigue,diarrheaand
pal-pable mass.2 Its origin is embryonic, developing from
postganglionic sympathetic nerve fibers, and it can be
associatedwithelevatedlevelsofcatecholamine’s.
Never-thelesshypertensionisuncommon,beingpresentin10---27%
http://dx.doi.org/10.1016/j.bjane.2014.07.012
0104-0014/©2014SociedadeBrasileiradeAnestesiologia.PublishedbyElsevierEditoraLtda.ThisisanopenaccessarticleundertheCC
Anestheticmanagementofaninfant 211
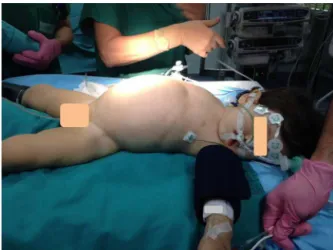
Figure1 Infantafteranestheticinduction.
ofcases.3Possiblemultiorganicaffectation,mainlyeffects
in cardiovascular and respiratory system, as well as the
treatmentofseverehypertensiondeservetobereviewed.
The parentsofthe patientgavewritteninformedconsent
forpublicationofthisarticle.
Case
report
A 15-month-old, 8.5kg boy was admitted on the
emer-gencydepartment of ourinstitution, withfatigue, partial
rejection of intake, weight loss, vomiting and abdominal
distension (Fig. 1). Laboratory testing revealed
hyper-uricemia (7.1mg/dL), hypoalbuminemia (3.2g/dL), LDH
4205.0IU/L, sodium 129.0mEq/L, potassium 3.5mEq/L,
chloride90.0mEq/L.AbdominalMRIshowedalarge
abdom-inalmass(12cm×10cm×10cm)encompassingmesentery
and retroperitoneum and compressed and displaced both
kidneys,surroundingcircumferentiallytheaortaandrenal
arteries and veins (Fig. 2). Persistent severe
hyperten-sionwaspresent(180---120mm/Hg).Echocardiographyruled
out the presence of associated heart disease.
Intra-venousinfusionofsodiumnitroprusside(0.5---3mg/kg/min)
was administered for acute blood pressure control. After
72h, sequential oral treatment was started with
cloni-dine (20mg/6h), nifedipine (4mg/6h) and propranolol
(3mg/8h),reachingastablemeanarterialpressuretarget
Figure2 AxialMRIshowsthegiantintraabdominalmass.
of 100mm/Hg. A MAPlower than 100mm/Hg determined
a critical decrease in tissue perfusion pressure reflected
withtheestablishmentofoligoanuria.Hewastakentothe
operatingroom for a series of biopsies (abdominal mass,
bone marrow and lymph nodes) to confirm the
diagno-sis.Rapid sequence induction wasperformed withSellick
maneuverafteradequatepreoxygenationwith100%oxygen,
andanesthesiainductionwithremifentanil(0.2g/kg/min),
propofol (2.5mg/kg), rocuronium (1.2mg/kg) and
lido-caine(1mg/kg).Trachealintubationproducednosignificant
changesin vitalsigns. The pressure-controlledventilation
was adjusted to maintain normocapnia using a mixture
of oxygen-air(FiO 50%). Maintenance of general
anesthe-sia was carried out using sevoflurane and remifentanil
(0.2---0.6g/kg/min).Persistedhypertensionwascontrolled
withestablishedantihypertensivetreatmentandincreasing
dosesof remifentanilduringthesurgery. Aftercompletion
of the surgical procedure infant was transferred to the
PICUmaintainingintravenousinfusionofsodium
nitroprus-side.Thediagnosisofneuroblastomawasconfirmed.Urine
catecholamine’s or their metabolites were undetectable.
Thesubsequentchemotherapyandtumorresectionallowed
restorationofnormalbloodpressure.
Discussion
Neuroblastoma derives from cells of neural crest, which
canbelocated at anyplacewhere thesearepresent and
theyretainthepotentialtosynthesizecatecholamines.Both
featuresaredeterminantsofassociatedpathophysiological
alterations.4
Itslocationisusuallyintraabdominal,althoughitis
pos-sible intrathoracic or cervical location and may produce
airway compromise. The presence of an abdominal mass
increases intra-abdominal pressure (IAP).1 This increases
therisk of aspirationtherefore, rapid sequence induction
is recommendable. In the respiratory system it
deter-minescephalicdisplacement of thediaphragm,increasing
intrathoracicpressureanddecreasinglungcomplianceand
functional residual capacity, which determines a greater
tendency to pulmonary atelectasis, impaired ventilation
perfusion ratio after induction of general anesthesia and
hypercapniaandhipoxemia.Itproducespulmonary
vasocon-strictionandincreasesthegasexchangeimpairmentinthe
alveolar-capillaryunit.Theextentofchangesinthe
cardio-vascularsystemisdependentonthemagnitudeoftheIAP,
presence of cardiomyopathy, intravascular volumestatus,
mode of mechanical ventilation, surgical conditions, and
anestheticagents employed.Systemic vascular resistance
increasesduetomechanicalcompressionoftheabdominal
aorta,highlevelsofneurohumoralfactorslikevasopressin, activationoftherenin---angiotensin---aldosteronesystemand
compressionoftherenalarteries,leadingtohypertension.
This high afterloadincreases the risk of acute pulmonary
edema. Compression of the inferior vena cava reduces
preloadandcardiacoutputdecreasingtissueperfusion,
par-ticularlyinpresenceofhypovolemia.Tachyarrhythmiasare
frequentduetohypercapnia andincreasedlevelsof
circu-latingcatecholamines.Allthesechangesmaydecreaseafter
laparotomyduetodecompressionoftheabdominalcavity,
212 M.Á.Gómez-Ríosetal.
Table1 Commondrugsusedtotreathypertensioninpediatricpatients.
Drug Routeof administration
Dose Notes
Clonidine PO 5---10g/kg24h(2---4doses) ␣2-adrenergicagonist.Riskofprolongedsedation. Nifedipine PO 0.25---0.5mg/kg4---6h Dihydropyridinecalciumantagonist.
Predominantlyvasculareffects. Propranolol PO/IV 0.05---0.2mg/kgiv
0.5---1mg/kg24h(3---4 doses)vo
Nonselectiveblockade.Riskofbronchospasm, myocardialdysfunction,AVblockand
hypoglycemia.
Labetalol IV 0.25---1mg/kg/h Nonselectiveblockade.Sideeffectsaresimilarto thoseofpropranolol.
Esmolol IV 50---200g/kg/min Relativelyselectiveblockade.Shorthalf-life (10min).
Sodium nitroprusside
IV 0.5---10g/kg/min Potentdirectrelaxationofvascularmuscletissue, botharteriolarandvenouscapacitancevessels. Potentialcyanidetoxicity;reflextachycardia. Nitroglycerin IV 0.5---10g/kg/min Directsmoothmusclerelaxation,predominantly
ofvenouscapacitancevessels.
Phentolamine IV 0.5---5g/kg/min Selectiveblocker,mainlyarteriolarvasodilation. Hydralazine IV 0.1---0.2mg/kg6h Directsmoothmusclerelaxation,predominantly ofarteriolar.Longhalf-life.Tachyphylaxis;reflex tachycardia;thrombocytopenia;lupus-like syndrome.
Urapidil IV Initially:2mg/kg/h Maintenance:0.8mg/kg/h. Max.7days
Electiveantagonistofperipheralpostsynaptic 1-adrenergicreceptors.
Enalapril PO/IV 0.1---0.5mg/kg24h(1---2 doses)PO
5---10g/kg8---24hiv
Angiotensinconvertingenzymeinhibitor.Effectof longduration.Hyperkalemia,renalfailure, angioedema;severehypotensionwithanesthetic agents.
PO,Orally;IV,intravenously.
Hypertension, in addition to the above mechanisms, can result from the vasoconstrictor action of cate-cholamines secreted by the tumor or the stimulation of the renin---angiotensin---aldosterone system secondary to compression of the renal artery. There may be an associated cardiomyopathy but it is uncommon. Its etiology is multifactorial3; it includes
catecholamine-induced vasoconstriction, coronary vasospasm, chronic
tachycardiomyopathysecondarytoahyperadrenergicstate,
b-adrenergicreceptors down regulation and promotion of
calciuminfluxintosarcolema.Effectivetreatmentof
hyper-tensionbeforesurgeryismandatorytoreduceperioperative
morbidityandmortality.Intraoperativehypertensive crisis
mayoccur,especiallyduringtrachealintubation,anesthetic
induction and tumor manipulation. Thus, it is critical to
minimize the sympathetic response secondary to direct
laryngoscopy.5 Thiopental, succinylcholine, and morphine
shouldbeusedwithcautionduetocatecholamine release
secondarytohistaminereleasefrommorphineorthiopental,
increased abdominal pressure or sympathetic stimulation
following succinylcholine.2 Intraoperative hypertension in
patients with catecholamine secreting neuroblastomas is
controlledusingshort-acting agents suchassodium
nitro-prusside,calciumantagonists,phentolamine,adenosineor
prostaglandinE1.2Theuseofantihypertensivedrugsin
pedi-atricpatients shouldbeinitiated in thelower dose under
close cardiovascular monitoring and titrated to effect.6,7
Table1showsthedrugscommonlyusedfortreating hyper-tensioninpediatricpopulation.
Management of patients with giant abdominal
neuro-blastoma is an anesthetic challenge. The knowledge of
pathophysiological implications and the adequate
antihy-pertensivetreatmentareessentialforsuccessfulanesthetic
management.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
References
1.HammerG,HallS,DavisPJ.Anesthesiaforgeneralabdominal, thoracic,urologic,andbariatricsurgery.Neuroblastoma proce-dures.In: Davis PJ,Cladis FP, Motoyama EK, editors.Smith’s anesthesiaforinfantsandchildren.8thed.Philadelphia:Elsevier Mosby;2006.p.754---5.
2.Seefelder C, Sparks JW, Chirnomas D, et al. Periopera-tive management of a child with severe hypertension from a catecholamine secreting neuroblastoma. Paediatr Anaesth. 2005;15:606---10.
Anestheticmanagementofaninfant 213
4.KainZN,Shamberger RS,HolzmanRS.Anestheticmanagement ofchildrenwithneuroblastoma.JClinAnesth.1993;5:486---91.
5.Kako H, Taghon T, Veneziano G, et al. Severe intraoperative hypertensionafterinductionofanesthesiainachildwitha neu-roblastoma.JAnesth.2013;27:464---7.
6.Cladis FP. Pediatric drug dosages. In: Davis PJ, Cladis FP, Motoyama EK, editors. Smith’s anesthesia for infants
and children. 8th ed. Philadelphia: Elsevier Mosby; 2006 [AppendixA].