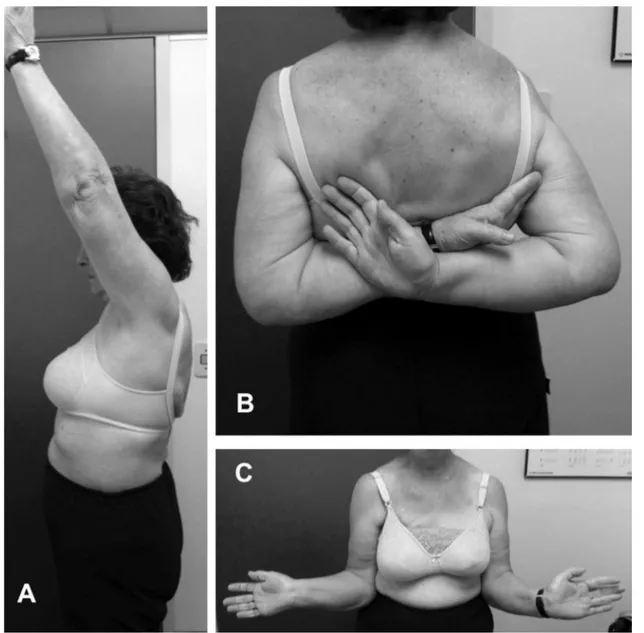
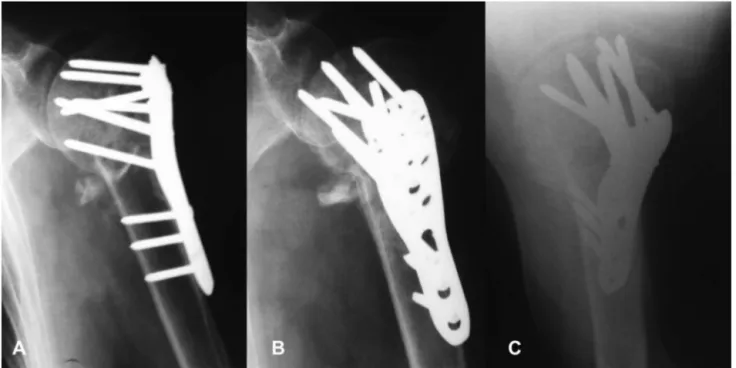
Rev. bras. ortop. vol.48 número6
Texto
Imagem
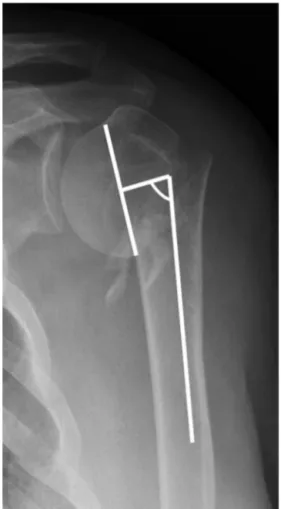

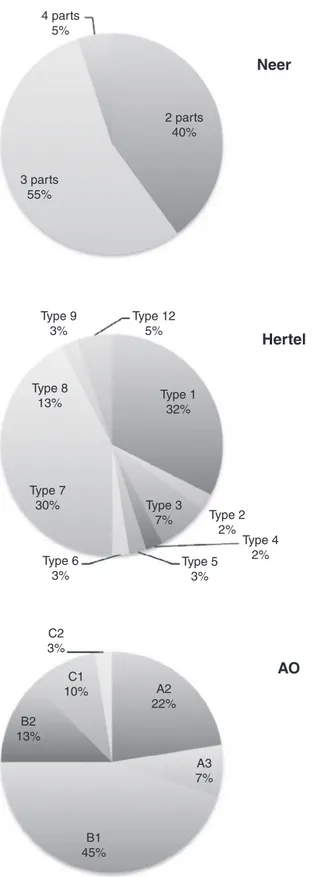
Documentos relacionados
Além disso, o Facebook também disponibiliza várias ferramentas exclusivas como a criação de eventos, de publici- dade, fornece aos seus utilizadores milhares de jogos que podem
Ousasse apontar algumas hipóteses para a solução desse problema público a partir do exposto dos autores usados como base para fundamentação teórica, da análise dos dados
i) A condutividade da matriz vítrea diminui com o aumento do tempo de tratamento térmico (Fig.. 241 pequena quantidade de cristais existentes na amostra já provoca um efeito
Na hepatite B, as enzimas hepáticas têm valores menores tanto para quem toma quanto para os que não tomam café comparados ao vírus C, porém os dados foram estatisticamente
Provar que a interseção de todos os subcorpos de E que são corpos de decomposição para f sobre F é um corpo de raízes fe
Despercebido: não visto, não notado, não observado, ignorado.. Não me passou despercebido
Universidade Estadual da Paraíba, Campina Grande, 2016. Nas últimas décadas temos vivido uma grande mudança no mercado de trabalho numa visão geral. As micro e pequenas empresas
Caso utilizado em neonato (recém-nascido), deverá ser utilizado para reconstituição do produto apenas água para injeção e o frasco do diluente não deve ser