r e v b r a s o r t o p . 2016;51(5):606–609
SOCIEDADE BRASILEIRA DE ORTOPEDIA E TRAUMATOLOGIA
w w w . r b o . o r g . b r
Case
Report
Bilateral
distal
femoral
fracture
after
total
knee
arthroplasty
夽
Fabrício
Bolpato
Loures
∗,
Jorge
Rafael
Wenck
Motta,
Rodrigo
Sattamini
Pires
e
Albuquerque,
João
Maurício
Barretto,
Naason
Trindade
Cavanellas
InstitutoNacionaldeTraumatologiaeOrtopedia(Into),CentrodeCirurgiadoJoelho,RiodeJaneiro,RJ,Brazil
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received12September2015
Accepted20October2015
Availableonline30August2016
Keywords:
Arthroplasty,knee
Femoralfractures
Elderly
a
b
s
t
r
a
c
t
Thenumberoftotalkneearthroplastieshasincreasedexponentiallyandtheirindications
havebeenexpanded.Thisprocedurepresentschallengingcomplicationsfororthopedic
surgeonsthatarepotentiallycatastrophicforpatients.Here,ararecaseofsimultaneous
bilateralperiprostheticfractureofthekneeisreported,withdiscussionofthecausalfactors,
possiblemanagementandprophylaxis.
©2016SociedadeBrasileiradeOrtopediaeTraumatologia.PublishedbyElsevierEditora
Ltda.ThisisanopenaccessarticleundertheCCBY-NC-NDlicense(http://
creativecommons.org/licenses/by-nc-nd/4.0/).
Fratura
bilateral
do
fêmur
distal
após
artroplastia
total
do
joelho
Palavras-chave:
Artroplastiadojoelho
Fraturasdofêmur
Idoso
r
e
s
u
m
o
Onúmerodeartroplastiastotaisdojoelhotemaumentadodeformaexponencialesuas
indicac¸õestêmsidoampliadas.Oprocedimentoapresentacomplicac¸õesdesafiadorasao
cirurgiãoortopédicoepotencialmentecatastróficasparaopaciente.Osautoresrelatamum
rarocasodefraturaperiprotéticadojoelho,bilateralesimultâneaediscutemosfatores
causais,aspossíveiscondutaseaprofilaxia.
©2016SociedadeBrasileiradeOrtopediaeTraumatologia.PublicadoporElsevierEditora
Ltda.Este ´eumartigoOpenAccesssobumalicenc¸aCCBY-NC-ND(http://
creativecommons.org/licenses/by-nc-nd/4.0/).
Introduction
Periprostheticfracturesofthekneeareararebutpotentially
devastating complication,1 representing a challenge to the
夽
StudyconductedatInstitutoNacionaldeTraumatologiaeOrtopedia(Into),RiodeJaneiro,RJ,Brazil.
∗ Correspondingauthor.
E-mail:[email protected](F.B.Loures).
orthopedicsurgeon.2Withthegrowthinthenumberoftotal
knee arthroplasties (TKA)each year, the frequency of this
complicationisincreasing.3Theincidencerangesinthe
lit-eraturefrom0.3%to4.2%forprimaryTKA1,4 andfrom1.6%
http://dx.doi.org/10.1016/j.rboe.2016.08.018
2255-4971/©2016SociedadeBrasileiradeOrtopediaeTraumatologia.PublishedbyElsevierEditoraLtda.Thisisanopenaccessarticle
rev bras ortop.2016;51(5):606–609
607
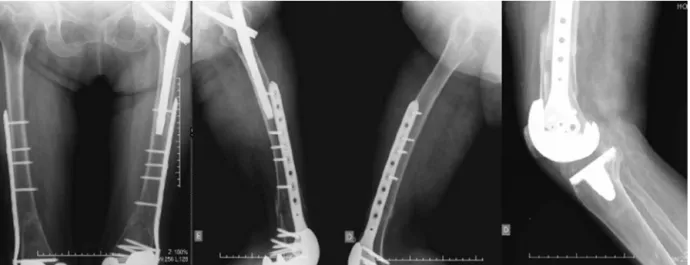
Fig.1–RadiographsafterTKAandfixationoftheproximalfemur.
to 38% for revisions.2,4 The most common mechanism of
injuryislow-energytrauma.However,elderlypatientshave
littlehemodynamicreserve,whichincreasesmorbidityand
mortality.2,3High-energytraumascanoccurin10%ofcases.5
Case
report
Female patient, 73 years old, white,retired, withsystemic
hypertension without other conditions, whose main
com-plaint was pain in both knees, worse on the right. She
presentedbilateralvarusknee;radiographicexamination
dis-closedgonarthrosis.Conservative treatmenthadbeen tried
foroverayear,butthepainremainedrefractory.
Sheunderwent TKA on the rightside on November 27,
2006.OnMay25,2008,shesuffered afallfrom ownheight
andwasadmittedforsurgicaltreatmentoftranstrochanteric
fractureontheleftfemur,fixedwithacephalomedullarynail.
OnAugust07,2009,sheunderwentontheleftside.She
pro-gressed without complications in all postoperative periods
andwas placedinoutpatientfollow-up forannual reviews
(Fig.1).
In2015,shesufferedanotherfallfromownheight,resulting
inbilateralsupracondylarfractureofthefemur(Fig.2),
clas-sifiedastypeIIinaccordancewiththeRorabeckandTaylor
criteria.6Sheunderwentsurgicaltreatmentforsimultaneous
fixation,withpolyaxiallockingplatesintroducedthroughthe
lateral subvastus approach in order to bridge the fracture
(Fig.3).
Thepatienthadanuneventfulrecoveryandconsolidation
occurredinthethirdpostoperativemonth(Fig.4).Sheis
cur-rentlyinoutpatientfollow-upandisabletowalkwiththeaid
ofacane.
Discussion
Thenumberofarthroplastieshasbeengrowingexponentially.
IntheUnitedStates,itisestimatedthatthisnumberincreases
by5%each year;this percentageishigher amongpatients
below65yearsofage.3
Despitebeingarelativelyrarecomplication,theincidence
of periprosthetic fractures is also increasing. Meek et al.2
reportedthattheabsolutefrequencyofthiscomplicationhas
doubledinScotlandbetween2001and2007;itisthefourth
causeofTKArevision.4Themostfrequentsiteofoccurrence
isthedistalfemur,followedbythepatellaandproximaltibia.
Theclassicpredisposingfactorsareosteopenia,infection
and osteolysis, female gender, older age, anterior femoral
notching,andrevisionarthroplasty.3 However,Singhetal.,1
inaretrospectivestudyof21,723arthroplasties,foundthat
the onlysignificantfactor forfracture inprimaryTKA was
608
rev bras ortop.2016;51(5):606–609Fig.3–Radiographsoftheimmediatepostoperativeperiod.
patient’sage.Thisincidenceshowedabimodaldistribution:
thefirstpeakwasbelow60years,andthesecond,above80
years.Theseauthorsdiscussedthelikelihoodofamoreactive
lifestyle amongyounger patients generating a higher
ten-sionatthebone-implantinterface.Thisgroupalsoincluded
patientswithinflammatorydiseases;duetothechronicuse
ofcorticosteroids,thesepatientshaveworsebonequality.
Anteriorfemoralnotchingisclassicallydescribedasa
pre-disposingfactortosupracondylarfemoralfracture.Although
biomechanicalstudieshavedemonstratedadecreasein
resis-tance, especially to torsional forces, clinical studies have
foundthisassociationdifficulttoprove.Ritteretal.7assessed
1,089casesofprimaryTKAandfoundanteriorfemoral
notch-ingin325ofthem(29.8%).Afterameanof5.1yearsfollow-up,
therewere twocasesofsupracondylarfracture,bothinthe
groupwithoutanteriorfemoralnotching.Thepresentpatient
hadasmallanteriorfemoralnotchingintheleftknee,butthe
authorsdonotbelievethereisacausalrelationshiptofracture.
Thetreatmentaimstorestorethepatient’s mobilityand
promotegoodfunctionthroughrecoveryofthelimb’slength,
alignment,androtation. Thestatusofthe implantfixation
shouldbeestablished;incaseofloosening(RorabecktypeIII),
TKArevisionmustbeperformed.3FortypeIandIIfractures,
therearetwofixationoptions:retrogradeintramedullarynail
andlockingplates.Carvalhoetal.5reportedacaseofbilateral
periprostheticfractureofthedistalfemurtreatedwith
retro-gradenail;consolidationoccurredinthefourthmonth.This
typeofnailrequiresaminimumdistalfragmentof2cm,which
wasobservedinCarvalhoetal.’scase,butnotinthepresent.
Althoughretrogradenailspresentadistinctadvantageinthe
preservationofsofttissueandgreaterconsolidationratio,
Her-reraetal.,8afterasystematicreviewof415cases,wereunable
toshowanadvantageofonefixationmethodovertheother.
Inthepresentcase,theauthorsoptedfortheuseof
polyax-ial lockingplate.Thisimplantallowsthepositioningofthe
lockingscrewsata30◦angle,leadingtobetterpositioningof
plateandbetterfixationofthefragments.Furthermore,the
useofretrogradenailwouldgenerateatensionpointwiththe
hipimplant,whichdidnotoccurduetotheoverlappingofthe
plateonthetipofthetrochantericnail.
The periprosthetic fracture is a challenge to the
ortho-pedicsurgeon, consideringtreatment,recovery, andrateof
complications.Althoughtherearefewdataintheliterature,
nonunionprevalencerangesfrom9%to20%;infection,from
rev bras ortop.2016;51(5):606–609
609
3%to 9%; loss ofthe reduction,from 4%to 27%; and the
incidenceofreoperationsisaround13%.8,9Sometypeof
com-plicationmaybepresentinover50%ofcases.9
Orthopedic surgeons who treat patients with severe
osteoarthritis of the knee generally have little interest in
investigatingbonequality,probablybecausetheincidenceof
osteoporosisislowerinpatientswithosteoarthritis.Chang
etal.,10afterevaluatingthebonedensityof347patients
under-goingTKA,allfemaleandover65years,foundanosteoporosis
prevalenceof31%,lowerthaninthecontrolgroup(42%).The
presentpatienthad awarningsignforosteoporosis,which
was the left proximalfemur fracture. Orthopedicsurgeons
mustbeawareofthispossibility,becausetreatingthe
underly-ingdiseasemayavoidapotentiallycatastrophiccomplication.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
r
e
f
e
r
e
n
c
e
s
1. SinghJA,JensenM,LewallenD.Predistorsofperiprosthetic fractureaftertotalkneereplacement.Ananalysisof21,723 cases.ActaOrthop.2013;84(2):170–7.
2. MeekRMD,NorwoodT,SmithR,BrenkelIJ,HowieCR.Therisk ofperi-prostheticfractureafterprimaryandrevisiontotal
hipandkneereplacement.JBoneJointSurgBr.2011;93(1): 96–101.
3.DavisN,HigginsG.Periprostheticfracturesaroundtotalknee arthroplasty.Trauma.2014;16(3):174–82.
4.ToogoodPA,VailTP.Periprostheticfractures:acommon problemwithadisproportionatelyhighimpactonhealthcare resources.JArthroplasty.2015;30(10):1688–91.
5.CarvalhoM,FonsecaR,SimõesP,BahuteA,Mendonc¸aA, FonsecaF.Bilateraldistalfemoralmailinginraresymmetrical periprosthetickneefracture.CaseRepOrthop.
2014;2014:745083.
6.RorabeckCH,TaylorJW.Classificationofperiprosthetic fracturescomplicatingtotalkneearthroplasty.OrthopClin NorthAm.1999;30(2):209–14.
7.RitterMA,ThongAE,KeatingEM,FarisPM,MedingJB,Berend ME,etal.Theeffectoffemoralnotchingduringtotalknee arthroplastyontheprevalenceofpostoperativefemoral fracturesandonclinicaloutcome.JBoneJointSurgAm. 2005;87(11):2411–4.
8.HerreraDA,GregorPJ,ColePA,LevyBA,JönssonA,Zlowodzki M.Treatmentofacutedistalfêmurfracturesaboveatotal kneearthroplasty.Systematicreviewof415cases(1981–2006). ActaOrthop.2008;79(1):22–7.
9.PlatzerP,SchusterR,AldrianS,ProsquillS,KrumboeckA, ZehetgruberI,etal.Managementandoutcomeof periprostheticfracturesaftertotalkneearthroplasty.J Trauma.2010;68(6):1464–70.
10.ChangBC,KimTK,KangYG,SeongSC,KangSB.Prevalenceof osteoporosisinfemalepatientswithadvancedknee