r e v b r a s o r t o p . 2013;48(6):578–580
w w w . r b o . o r g . b r
Case
Report
Osteochondritis
dissecans
in
bilateral
lateral
femoral
condyle
in
knees
夽
Ari
Zekcer
a,
Ricardo
Soares
da
Silva
a,∗,
Renato
Akira
Iwashita
a,
Mario
Carneiro
Filho
baKneeSurgerySector,TatuapéOrthopedicsClinic,Taubaté,SP,Brazil
bDepartmentofOrthopedicsandTraumatology,EscolaPaulistadeMedicina,UniversidadeFederaldeSãoPaulo,SãoPaulo,SP,Brazil
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received30September2012 Accepted15January2013
Keywords:
Osteochondritisdissecans Knee
Cartilagearticular
a
b
s
t
r
a
c
t
Theosteochondritisdissecans(OCD)isadiseaseofunknowncausethatclassicallyaffects thekneelateralborderofthemedialfemoralcondyle.WepresentararecaseofOCDin bilaterallateralfemoralcondyle.
©2013SociedadeBrasileiradeOrtopediaeTraumatologia.PublishedbyElsevierEditora Ltda.Allrightsreserved.
Osteocondrite
dissecante
em
côndilo
femural
lateral
bilateral
nos
joelhos
Palavras-chave:
Osteocondritedissecante Joelho
Cartilagemarticular
r
e
s
u
m
o
Aosteocondritedissecante(OCD)éumapatologiadecausadesconhecida,que classica-menteacometenojoelhoabordalateraldocôndilofemuralmedial.Apresentamosumraro casodeOCDnocôndilofemurallateralbilateral.
©2013SociedadeBrasileiradeOrtopediaeTraumatologia.PublicadoporElsevierEditora Ltda.Todososdireitosreservados.
Case
report
Thepatientwasa28-year-oldwhitefemalenurseof seden-tary habits who presented a complaint of sudden pain in her left knee around 20 days earlier, without any history oftrauma.Theconditionimprovedwithnon-steroidal anti-inflammatorydrugsandworsenedafterphysicalexertion.She alsoreportedthatshehadhadasimilarconditioninherright
夽
WorkperformedattheTatuapéOrthopedicsClinic,Taubaté,SP,Brazil. ∗ Correspondingauthor.
E-mail:ricardoortop@hotmail.com(R.S.daSilva).
kneethreeyearsearlier,buttherightkneewasasymptomatic atthistime.
On physical examination, she presented bilateral genu valgum with crepitation on flexion–extension and pain on anterolateral palpation in both knees.The pain was more intenseintheleftknee,whichalsopresentedeffusion(+/4+). RadiographsinAP,lateraland tunnelviewswere produced onthepatient,andalsobilateralmagneticresonance imag-ing (MRI). This revealed unstable osteochondral fragments
rev bras ortop.2013;48(6):578–580
579
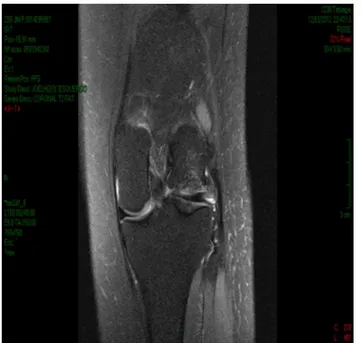
Figure1–PreoperativeMRIontheleftknee.
measuring30mm×20mminthelateralfemoralcondylein
theleftkneeand30mm×28mmintherightknee.
Accord-ingtotheInsallclassificationforMRIonosteochondritis,1the
lesionswereclassifiedasstageVontheleftsideandstageIV ontherightside(Figs.1and2).
Weimplemented surgicaltreatment initiallyon the left knee.Thepatientunderwentarthroscopywithjoint inspec-tion, in which we observed a chondral lesion of around 30mm×20mminthelateralfemoralcondyleoftheleftknee,
withaloosechondralfragmentinthejoint.Thisfragmentdid notpresentvitalityandwasofivoryappearance,andinsitu fixationwascontraindicated.Wethenperformedarthrotomy, withexposureofthelateralcondyleofthefemur.Wedecided toperformmosaicplasty,usinganautologousosteochondral graft. This was obtained by removing three osteochondral plugsfromthelateralfaceofthetrochleaofthelateralfemoral condyle(donorzone),usingtrephineswithan8mmArtrex® guide(Fig.3),inordertofilltheinjuredarea(recipientzone). Thepatientwasdischargedfromhospitalonedayafterthe
Figure2–PreoperativeMRIontherightknee.
Figure3–PostoperativeMRIontheleftknee.
surgery, without immobilization, but shecontinued to use crutchesfor45days,withoutweight-bearing,andwithpassive range-of-motionexercises.Herconditionevolved satisfacto-rily,withoutpainorlimitations.
Oneyear afterthe surgeryon theleft knee, the patient startedtocomplainofpainandjointlockingintherightknee. She then underwent surgical treatment with arthroscopy, which showed the lesion in the lateral femoral condyle and the presence of a free intra-articular body measuring around 30mm×30mm. We performed lateral arthrotomy,
withremovaloftheloosefragment,andmosaicplastyonthe lateralfemoralcondyle,inwhichthreeosteochondralplugs wereremovedfromthedonorzoneonthelateralfaceofthe trochlea,inthesamewayasdoneintheprocedureontheleft knee.However,thistime,theplugswereofdiameter10mm andweusedtrephineswithaJohnson&Johnson®guide.We thenusedthesamepostoperativeprotocol,withsatisfactory evolution(Fig.4).
Oneyearandsixmonthshasnowpassedsincethe opera-tionontheleftknee,andsixmonthssincetheoperationon therightknee,andthepatientdoesnothaveanycomplaints orlimitations.
Discussion
Osteochondritisdissecans(OCD)isapathologicalcondition ofunknowncausethatoccursinthesubchondralbone.2,3It
presentsinajuvenileform,whenthegrowthplateisopen, orinanadultform,whenitispresentinthemature skele-ton.Thelattergenerallyrequiressurgicaltreatmentandhas worseprognosis.Clinically,itpresentsseveralformsof mani-festation.
Itclassicallyaffectsthelateralborderofthemedialfemoral condyle.2Bilateraloccurrenceandcasesinthelateralfemoral
580
rev bras ortop.2013;48(6):578–580Figure4–PostoperativeMRIontherightknee.
Itisclassifiedinaccordancewiththeanatomicallocation, stabilityofthefragmentandalterationsseenonMRI, scintig-raphyandradiographs.2 Alterationsseen inimagingaid in
choosingthetherapyand,whenthisisthecase,inthe evolu-tionofconservativetreatment.3
Thesurgical treatmentcomprises several techniques,4–8
such as resection of the fragment, arthroscopic drilling, mosaicplasty,insitufixationofthefragmentand microfrac-turing,amongothers,accordingtothelocationandviabilityof thefragment.9However,initialarthroscopyhasbeenshown
to beimportant forevaluating the type and extent ofthe lesionandthemobilityoftheosteochondralfragment.Ithas adirectimplicationinthechoiceofappropriatetherapyand inperformingitarthroscopicallywhenpossible.Arthrotomy canalsobechosen,whennecessary.10In thepresent case,
afterperformingarthroscopyandassessingthevitalityofthe fragmentanditssize,wedecidedtousemosaicplasty.
In this manner, we have reported a rare bilateral case ofosteochondritis dissecansofthe lateralfemoralcondyle, whichwastreatedbymeansofthemosaicplastytechnique withgoodclinicalresults.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
r
e
f
e
r
e
n
c
e
s
1.HeftiF,BerguiristianJ,KrauspaeR,Möller-MadsenB,RiccioV, TschaunerC,etal.Osteochondritisdissecans:amulticenter studyoftheEuropeanPediatricOrthopaedicSociety.JPediatr OrthopB.1999;8(4):231–45.
2.GanleyTJ,FlynnJM.Osteochondritisdissecans.In:ScottWN, editor.Surgeryoftheknee.4thed.NewYork:Churchill Livingstone;2006.p.1234–41.
3.AndersonAF,LipscombAB,CoulanC.Antegradecurettement, bonegrafting,andpinningofosteochondritisintheskeletally matureknee.AmJSportsMed.1990;18(3):254–61.
4.CetikO,TurkerM,UsluM.Bilateralosteochondritisdissecans oflateralfemoralcondyle.KneeSurgSportsTraumatol Arthrosc.2005;13(6):468–71.
5.GreenWT,BanksHH.Osteochondritisdissecansinchildren. ClinOrthopRelatRes.1990;(255):3–12.
6.HavulinnaJ,JokioP,LindholmTS,ViljanenV,SavilahtiS. Long-termresultsofSmilliepinfixationofosteochondritis dissecansinthefemoralcondyles.AnnChirGynaecol. 1995;84(1):71–80.
7.LindholmS,PylkkänenP.Internalfixationofthefragmentof osteochondritisdissecansinthekneebymeansofbonepins. Apreliminaryreportonseveralcases.ActaChirScand. 1974;140(8):626–9.
8.SloughJA,NotoAM,SchmidtTL.Tibialcorticalbonepeg fixationinosteochondritisdissecansoftheknee.ClinOrthop RelatRes.1991;(267):122–7.
9.TwymanRS,DesaiK,AichrothPM.Osteochondritisdissecans oftheknee.Along-termstudy.JBoneJointSurgBr.
1991;73(3):461–4.
10.SeverinoNR,CamargoOPA,AiharaT,CuryRPL,VazCES,Perez GG,etal.Osteocondritedissecantedojoelho:estudo