w w w . r b h h . o r g
Revista
Brasileira
de
Hematologia
e
Hemoterapia
Brazilian
Journal
of
Hematology
and
Hemotherapy
Case
Report
Idiopathic
hypereosinophilic
syndrome
with
20
years
of
diagnostic
delay
Miguel
Pedro
de
Queiroz
Neto
∗,
Fernando
Antônio
Galvão
Gondim
Filho
HospitalMetropolitanoNorteMiguelArraes(HMA),Paulista,PE,Brazil
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received5November2015 Accepted4November2016 Availableonline24January2017
Introduction
Eosinophils are specialized granulocytes that produce and store diverse biologically active molecules, including cyto-toxins, cytostimulatory proteins, lipid mediators, chemo-tactic peptides, cytokines, leukotriens and prostaglandins.1
Eosinophilscanalsocausedirectdamagetomicroorganisms and can activate cells and platelets.1,2 The normal count
rangesbetween0.05and0.5×109/Lintheperipheralblood
andbetween1%and6%inamyelogram.3
Hypereosinophilia is defined as persistent eosinophilia (>1.5×109/L) over a minimum of four weeks.3,4 Major
causes of hypereosinophilia are helminth infections, aller-gies, atopy and drugs, which are described as secondary hypereosinophiliaduetotheproductionofinterleukin (IL)-3andIL-5thatpromoteeosinophilproliferation.Lymphomas, lymphoblasticleukemia,somesolidtumorsandsome autoim-mune diseases are less common causes.3–5 In primary
hypereosinophilia,eosinophilsareclonalandarederivedfrom
∗ Correspondingauthorat:HospitalMetropolitanoNorteMiguelArraes(HMA),EnfermariadeClínicaMédica,EstradadaFazendinha,S/N,
53413-000Paulista,PE,Brazil.
E-mailaddress:[email protected](M.P.Neto).
myeloid lineage. Althoughrare, the maincausesare myel-ogenous leukemias and myelodysplasticsyndromes.3,4 The
clinical course varies as it may involve single or multiple organs. Thereare noclearimmunophenotypicmarkersfor clonalhypereosinophilia;however,therearehighlyindicative molecularmarkers.6Themostcommonareplatelet-derived
growthfactorreceptoralphaandbeta(PDGFR␣andPDGFR), fibroblastgrowthfactorreceptor1(FGFR1),thec-abl1 onco-gene(ABL1)andJanuskinase2(JAK2);thefirstthreearerelated tot(8;13),t(5;12)andt(9;22)cytogenetictranslocations.3,4,7
For a diagnosis of hypereosinophilic syndrome, tar-get organ damage, hypereosinophilia and absence of any other reason for organ damage are needed.6 Treatment is
basedonglucocorticoidsandnonsteroidalanti-inflammatory drugsaccordingtosymptoms,andtyrosine-kinaseinhibitors directedagainstcytogenetictargets.3,7,8
Herein,wereport acaseofhypereosinophilicsyndrome diagnosed as chronic myeloid leukemia with eosinophilia (CML-eo)inapatientwithsymptomsover20years.
http://dx.doi.org/10.1016/j.bjhh.2016.11.008
Figure1–AandBbeforeImatinib.
Case
report
A 30-year-old male patient presented to the emergency department with dyspnea, fever and productive cough for threedays.Hehad been taking20mgofprednisonefor20 years afterbeing admitted toa hospitalin Recife.On this occasion,thepatientwastreatedforstreptococcal glomeru-lonephritis.Afterdischarge,hedidnotreturnandwaslostto follow-up.
Thepatientalsohadpruriticskinlesionssincetenyearsof age,whichusedtoerupt,vanishandreappearspontaneously intwo-weekintervals.Afterprednisonewasstarted,the fre-quencyofthelesionswasrelatedtoitsintake,asthefrequency oflesionreappearancewasmuchhigherwithoutprednisone. Atphysicalexamination,thepatient’sheartratewas108 beatsperminute,respiratoryratewas28breathsperminute and the blood pressure was 180/100mmHg. He presented withcushingoidfacies, kneearthritis, violetstreaksonthe abdomenanddarkened skinwitherythematousand papu-larlesionsonhisface,limbsandtrunk(Figure1).Hehadno kidneyinjury,hepatomegalyorsplenomegaly.
Ceftriaxone and azithromycin were prescribed to treat communitary pneumonia and the prednisone dosage was reducedto15mg/day.
Onthefollowingdays,pustulesanderythrodermaaroseat previousskinlesionsites.Eosinophiliawasseeninperipheral bloodatlevelsabove6.0×109/L,whichwas30–50%ofthetotal
cellularity.Blastswerenotseeninperipheralblood.
Anti-neutrophilcytoplasmicantibody(ANCA),skinbiopsy, myelogramand humanimmunodeficiency virus (HIV)tests were examinedtoinvestigate secondaryhypereosinophilia.
TheANCAandHIVresultswerenegative.Theskinbiopsy diag-nosed eosinophilicpustular folliculitis and the myelogram revealed 20%eosinophilsinbonemarrow,with normoblas-tic erythropoiesis, normocellular granulopoiesis, 1% blasts andnormoblasticmegakaryocytes.Abdomenandthorax com-putedtomographywerealsoobtained,whichrevealedaxillary, cervicalandinguinallymphadenomegaly.
As an additional workup, no lymphocyte clonality was foundbyflowcytometry.Asubsequentmolecularpanelfor FIP1L1-PDGFR␣, breakpoint cluster region-Abelson murine leukemia (BCR-ABL) and JAK2 was obtained, showingonly BCR-ABLtranslocationaspositive.
After the recent diagnosis of eosinophilia-associated chronic myeloid leukemia (Eos-CML), hydroxyurea (2g/day) wasgivenandtheperipheralbloodeosinophiliawaspartially controlled.Thepatientdidnottolerateprednisonewithdrawal duetoanadrenalcrisisandhewasdischargedon15mg/day prednisone.Duringthefollow-up,imatinib(400mg/day)was prescribedandafterfivedaysoftreatment,theskinlesions receded. Scar spots remained in place of previous lesions (Figure2).
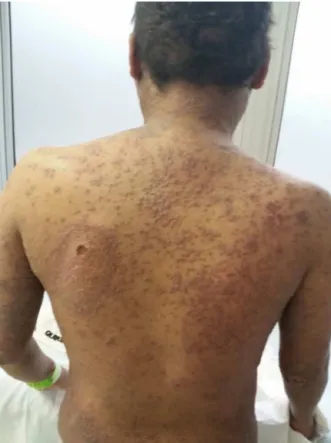
Afterfourweeksofimatinib,skinlesionsrelapsed.This timetherewerepustulesandulcersoftheoralmucosa,and ontheelbowsandback(Figure3).Thepatientalsocomplained aboutdysphagia,intensepruritusandoccasionaldyspnea,the latterwas alleviatedwithsalbutamolandthe prurituswas relieved with dexchlorpheniramine. The patient was read-mittedduetointensedysphagia.Acompletebloodcounton admissionshowed90.0×109/Lleukocytesofwhich80%were
Figure2–AandBafterImatinib.
couldnotbecontrolledevenwithapulsedoseof methylpred-nisolone.Anewmolecularpanelwasobtainedfromtissueand bloodexamswererepeated.
Skinbiopsyrevealedhypereosinophiliculcerationandthe entireskinmolecularpanelwas negative.TdT,CD89, c-kit, CD20, CD3, CD7, CD2, CD15, CD34, myeloperoxidase and
Figure3–Skinlesionsrelapse.
mutations of PDGFR were tested. The pathologist con-cludedthatthetissuewasinfiltratedbyanundifferentiated myeloproliferative neoplasm. Blood BCR-ABL and muta-tions of PDGFR were also negative. Another myelogram showed hypercellular bone marrow with 78% of cells being granulocytes (27% eosinophils and 51% eosinophil precursors)ofhypoblasticerythroidlineageand hypercellu-lar megakaryocyte lineage, presenting monolobulation and polylobulation.Animmunophenotypingpanelshowed hyper-cellularity,matureandintermediateeosinophilsconcludingit wascompatiblewithchronicmyeloproliferativeneoplasm.No cytogeneticstudyorbonemarrowbiopsywasmade.Asthe BCR-ABLresultswerediscrepant,anothersearchforBCR-ABL andPDFGRmutationswasmade,althoughtheresultswere negative.
Due to failure of tyrosine kinase inhibitor treatment andthenegativeBCR-ABLresults,imatinibwasceasedand hydroxyurea restarted with cellularity control. During the hospitalstay, thedyspneaworsening andanewthoraxCT was performed,whichrevealed a7.0cmdiametercavityin the righthemithorax. Itwas decidedtostarttreatmentfor tuberculosis with rifampicin, isoniazid, pyrazinamide and ethambutol.Despitethistherapy,thedyspneaworsenedand the patientstarted withfever.Bloodcultureswere positive to multidrug resistant Acinetobacter baumannii and Candida albicans.Subsequently,polymyxinB,gentamicinand micafun-gintherapywerestarted.
Thepatientbecamesepticandlaterdied.
Discussion
Table1–WorldHealthOrganizationdiagnosticcriteria forchroniceosinophilicleukemia.10
1.Eosinophiliacount≥1.5×109/L
2.ThereisnoPhiladelphiachromosomeorbreakpointcluster region-Abelsonmurineleukemia(BCR-ABL)fusiongeneorother myeloproliferativeneoplasm(polycythemiavera,essential thrombocythemia,orprimarymyelofibrosis)or
myelodysplastic/myeloproliferativeneoplasms(MDS/MPN) (chronicmyelomonocyticleukemia,atypicalchronicmyeloid leukemia)
3.Thereisnot(5;12)(q31–35;p13)oranyotherrearrangementof PDGFR
4.ThereisnoFIP1L1-PDGFR␣fusiongeneoranyother rearrangementofPDGFR␣
5.ThereisnorearrangementofFGFR1
6.Theblastcellcountinperipheralbloodandbonemarrowis <20%andthereisnoinv(16)(p13.1;q22)ort(16;16)(p13.1;q22)or otherdiagnosticfeatureofacutemyeloidleukemia
7.Thereisaclonalcytogeneticormoleculargeneticabnormality orblastcellsare>2%inperipheralbloodor>5%inbonemarrow
annualdischargesandonaUSdatabaseforoutpatient man-agement has indicated that hypereosinophilic syndromes couldrepresentapproximatelyone-thirdofchronicmyeloid leukemiapatients. However,other internationalreportsare relatedtoPDGFR mutations,whichare morecommon and predominantlyaffectmenwithanestimatedmale-to-female ratiobetween4:1and9:1withatendencytooccurinpeople agedfrom20to50yearsold.7,8
Theclinicalmanifestationsvaryvastly.Anyorganor tis-suemaybeaffectedandmyalgia,arthritis,dyspnea,pruritus, skinlesionsandothersymptomsmaydevelop.3,4,6Inthiscase,
themainclinicalmanifestationwaseosinophilicfolliculitis, whichischaracterizedbypruriticperifollicularerythematous papules and pustuleson the head, neck, limbsand trunk. Thereisnodataregardingitsprevalenceinhypereosinophilic syndromesorinmyeloproliferativeneoplasmsinthe litera-ture.However,skininvolvementiscommonandtherecanbe ulcerations.7
The World Health Organization (WHO) proposed a set of criteria to classify myeloproliferative neoplasms, for which molecular and cytogenetic data are required.9
Fol-lowing these criteria rigorously, the above case can only bediagnosed as idiopathic hypereosinophilic syndrome as thereisstrongevidenceofmyeloproliferativeneoplasm,but eosinophilclonalitycannotbeproventhroughmolecular stud-ies.Nonetheless,otherdiagnoseswouldbepossibleifthere wasflexibilityinthecriteria.Chroniceosinophilicleukemia, forexample,wouldbeastrongpossibilityinthiscasehowever, theabsenceofclonalitydidnotallowthisdiagnosis(Table1). Hence,the consensusofthespecialistswho addressedthis caseagreedthatthe WHOcriteriaareflawedand thatnew histopathologicandmorphologiccriteriashouldbedefinedto simplifythediagnosisinsituationsinwhichclonalitycannot beproven.4InthemostrecentWHOeosinophiliareview,no
diagnosticcriteriawerechanged.3Itisimportanttonotethat
nocytogeneticstudywasdoneinthiscase.
Anotherhypothesisinthiscasewaschronicneutrophilic leukemia.Amongtheeightcriteriaforthisdisease(Table2), thepatientdidnothavehepatosplenomegaly.TheWHOis rig-orousinthisdiagnosis perhapsbecausethis diseaseisstill
Table2–TheWorldHealthOrganizationdiagnostic criteriaforchronicneutrophilicleukemia.10
1.Peripheralbloodleukocytosis≥25.0×109/L,segmented
neutrophilsandbandformsare>80%ofwhitebloodcells, immaturegranulocytes(promyelocytes,myelocytes,
metamyelocytes)are<10%,myeloblastsare<1%ofwhiteblood cells
2.Hypercellularbonemarrowbiopsy,neutrophilicgranulocytes increasedinnumberandpercentage,myeloblasts<5%of nucleatedbonemarrowcells,neutrophilicmaturationpattern normal,megakaryocytesnormalorleftshifted
3.Hepatosplenomegaly
4.Noidentifiablecauseforphysiologicneutrophiliaor,ifpresent, demonstrationofclonalityofmyeloidcellsbycytogeneticor molecularstudies,noinfectiousorinflammatoryprocess,no underlyingtumor
5.NoPhiladelphiachromosomeorbreakpointcluster region-Abelsonmurineleukemia(BCR-ABL)fusiongene 6.NorearrangementofPDGFR␣,PDGFRorFGFR1
7.Noevidenceofpolycythemiavera,essentialthrombocythemia orprimarymyelofibrosis
8.Noevidenceofmyelodysplasticsyndromeor
myelodysplastic/myeloproliferativeneoplasms(MDS/MPN),no granulocyticdysplasia,nomyelodysplasticchangesinother myeloidlineages,monocytes<1.0×109/L
poorlycharacterized,asitreportsthatonly40ofthe150cases describedintheliteraturemetthecriteria.9
Inthiscase,thelongdurationofsymptomsandlackof dis-easeprogressionshouldberemembered.Theindiscriminate useofprednisonebythepatientmayalsohaveinfluenced dis-easeprogression.Anotherpossibilitythatshouldbetakeninto considerationisthatsincechildhood,thispatienthada hyper-eosinophilicsyndromethatevolvedintoamyeloproliferative neoplasm.
Conclusion
InitiallytreatedasCML-eoduetothelaboratoryfindings,this casepresentedthediagnosisofidiopathichypereosinophilic syndrome withthepatientevolving toanunfavorable out-come after presenting symptoms for 20 years prior to diagnosis.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
r
e
f
e
r
e
n
c
e
s
1.GleichGJ.Mechanismsofeosinophil-associatedinflammation. JAllergyClinImmunol.2000;105(4):651–63.
2.HoganSP,RosenbergHF,MoqbelR,PhippsS,FosterPS,LacyP, etal.Eosinophils:biologicalpropertiesandroleinhealthand disease.ClinExpAllergy.2008;38(5):709–50.
3.GotlibJ.WorldHealthOrganization-definedeosinophilic disorders:2014updateondiagnosis,riskstratification,and management.AmJHematol.2014;89(3):326–37.
classificationofeosinophilicdisordersandrelatedsyndromes. JAllergyClinImmunol.2012;130(3):607-12.e9.
5.MontgomeryND,DunphyCH,MooberryM,LaramoreA,Foster MC,ParkSI,etal.Diagnosticcomplexitiesofeosinophilia.Arch PatholLabMed.2013;137(2):259–69.
6.ValentP,HornyHP,BochnerBS,HaferlachT,ReiterA. Controversiesandopenquestionsinthedefinitionsand classificationofthehypereosinophilicsyndromesand eosinophilicleukemias.SeminHematol.2012;49(2):171–81.
7.MedvesS,DemoulinJB.Tyrosinekinasegenefusionsincancer: translatingmechanismsintotargetedtherapies.JCellMol Med.2012;16(2):237–48.
8.RoufosseFE,GoldmanM,CoganE.Hypereosinophilic syndromes.OrphanetJRareDis.2007;2:37.
9.VardimanJ,HyjekE.Worldhealthorganizationclassification, evaluation,andgeneticsofthemyeloproliferativeneoplasm variants.HematolAmSocHematolEducProgram.