jcoloproctol(rioj).2015;35(1):72–75
w w w . j c o l . o r g . b r
Journal
of
Coloproctology
Technical
Note
Endoscopic
pilonidal
sinus
treatment
(E.P.Si.T.):
a
minimally
invasive
approach
夽
Carlos
Ramon
Silveira
Mendes
a,b,c,∗,
Luciano
Santana
de
Miranda
Ferreira
a,c,
Ricardo
Aguiar
Sapucaia
a,c,
Meyline
Andrade
Lima
a,caColoproctologyService,HospitalSantaIzabel,SantaCasadeMisericórdiadaBahia,Salvador,BA,Brazil bHospitalGeralRobertoSantos,Salvador,BA,Brazil
cSociedadeBrasileiradeColoproctologia(SBCP),RiodeJaneiro,RJ,Brazil
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received3November2014 Accepted30November2014 Availableonline28January2015
Keywords:
Pilonidaldisease Pilonidalsinus Fistuloscope
a
b
s
t
r
a
c
t
Introduction:Thepilonidalcystisachronicinflammatoryprocessthatoccursfrequently inthesacrococcygealregion.Itismorecommoninmaleswitharatioof3:1andusually presentsitselfinthethirddecadeoflife.Thetreatmentismainlysurgicalwithvariousforms. Thesearchfornewtechnologiesaswellasforaminimallyinvasivetreatmenthasbecome ofutmostimportanceinsurgicalroutines.ThetechniqueE.P.Si.T.(endoscopictreatmentof pilonidalcyst)developedbyMeneirohasbeenquiteinterestinginthetreatmentofpilonidal cysts.
Surgicaltechnique:Anesthetizedthepatientinthesupineposition.Identifiedthedrainage holeofthecyst,andbeganwiththepassageoffistuloscopestudyingthepathofthecyst. Performsfollowingtheremovalofallthetissueinsideasthehairfollowedbycauterization ofthepath.Removedalldevitalizedtissueandenlargementoftheopeningofthecyst.
©2015SociedadeBrasileiradeColoproctologia.PublishedbyElsevierEditoraLtda.All rightsreserved.
Tratamento
endoscópico
do
cisto
pilonidal
(E.P.Si.T.):
Uma
abordagem
minimamente
invasiva
Palavraschave:
Doenc¸apilonidal Cistopilonidal Fistuloscopio
r
e
s
u
m
o
Introduc¸ão:Ocistopilonidaléumprocessoinflamatóriocrônicoqueocorrecomfrequência naregiãosacrococcígea.Émaiscomumnosexomasculinocomproporc¸ãode3:1emais presentenaterceiradécada.Otratamentoéeminentementecirúrgicocomdiversas for-masderealizac¸ão.Abuscadenovastecnologiasbemcomootratamentominimamente invasivosetornouprioridademáximanasrotinascirúrgicas.AtécnicadoE.P.Si.T (Trata-mentoendoscópicodocistopilonidal)desenvolvidaporMeneirotemsemostradobastante interessantenotratamentodoscistospilonidais.
夽
StudyconductedatHospitalSantaIzabel,SantaCasadeMisericórdiadaBahia,Salvador,BA,Brazil. ∗ Correspondingauthor.
E-mail:proctoramon@hotmail.com(C.R.S.Mendes). http://dx.doi.org/10.1016/j.jcol.2015.01.007
jcoloproctol(rioj).2015;35(1):72–75
73
Técnicacirúrgica:Pacienteemdecúbitodorsalsobanestesia.Identificaoorifíciodedrenagem docisto,einiciacomapassagemdofistuloscópioestudandootrajetodocisto.Realizaa seguiraremoc¸ãodetodootecidonointeriorcomoosfiosdecabeloseguidodacauterizac¸ão dotrajeto.Removidotodootecidodesvitalizadoeampliac¸ãodaaberturadocisto.
©2015SociedadeBrasileiradeColoproctologia.PublicadoporElsevierEditoraLtda. Todososdireitosreservados.
Introduction
Pilonidalcystisachronicinflammatoryprocessthatoccurs withfrequencyinthesacrococcygealregion,usually associ-atedwiththepresenceofhairinthisregion.1–6Itspresentation
ismorecommoninmales,witharatioof3:1,usuallyinthe thirddecadeoflife.7,8
Themethods usedforpilonidal cysttreatmentare emi-nentlysurgical.Severalformsaredescribed,suchasincision andcurettageandexcisionandflaprotation,aswellas exci-sionwithsecondintentionhealing.9–11Theseapproachesare
quite aggressive, resulting in a large wound that must be caredfor.Withtheadventofnewtechnologiesandthe pur-suitforminimallyinvasiveprocedures,Meneirodescribedin 2013anapproachforendoscopictreatmentofpilonidalcysts (E.P.Si.T.).12Thisprocedurewasdevelopedaftertheuseofa
fis-tuloscopeforanalfistulas,13,14beingappliedtothispathology.
Theaimofthisstudyistodescribethefirstreportofthis techniqueinBrazil,heldbyourteam,inJune2014.
Surgical
technique
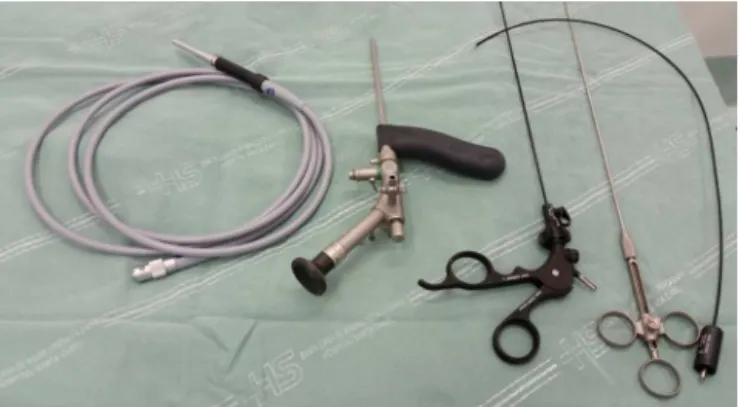
Toperformtheprocedure,aspinalanesthesiaisrequired;the patientisplacedinaventralrecumbentposition,with iden-tificationoftheorificeofcystdrainage.Thesurgeonstands betweenthepatient’slegsandthevideosetispositionedto theleftofthesurgeon(Fig.1).Toperformthe technique,a kit,whichincludesthefistuloscope(KarlStorzGmbH, Tuttlin-gen,Germany;Fig.2),anobturator,anendobrush,aunipolar electrodeandagraspingforceps,isused.The18-cmlength fis-tuloscopehasan8◦angledeyepiece;thedevicehasadiameter of3.2mm×4.8mm,beingconnectedtoanopticalfiberandto acontinuousirrigationsystem.Afterthepassageofthe fis-tuloscopethroughthecystholewithinfusionof1%glycine
Fig.1–Introductionofthefistuloscope.
ormannitol,thesurgeonsearchesthecyst,lookingfor acces-sorytractsaswellasforabscesses.Oncetheobturatorofthe equipmentisremoved,thesurgeonstartsremovinghairand devitalizedtissues.Afterstudyingthecystandfinishingthe tissueremoval,thewhole-tractcauterizationstagebegins.To thatend,thesurgeonusestheelectrocauteryconnectedtoa powersourcetoremoveallgranulationtissuepresentinthe cystcavity.Necrotictissueisremovedwithbrushingthe cav-ity;withthat, thewholetractiscleaned.Attheendofthe procedure,thesurgeoncreatesanexternalopeningto facili-tatedrainageofthecavity,andalsotoenlargetheinitialhole (Fig.3).
Discussion
Pilonidalcystisaverycommondisorder,withanestimated incidenceof26casesper100,000people,affectingmenthree timesmorethanwomen.15Menaremoreaffectedthanksto
Fig.2–Fistuloscope,KarlStorzGmbH(Tuttlingen, Germany).
74
jcoloproctol(rioj).2015;35(1):72–75their naturalhirsutism. The occurrenceof apilonidal cyst isalsoassociatedwithobesity,sedentarylifestyle andlocal irritationor trauma.16,17 The treatment ofpilonidal cyst is
mainlysurgical;therearevarioustechniquesdescribedinthe literature,e.g., incision and curettage, excision, techniques combinedwithplasticsurgerywithrotationflaps, marsupi-alizationorfistulotomy.18Theidealmethodshouldcombine
asmallerlossoftissue,minimalpostoperativemorbidity, cos-metic results,rapidreturn towork activities, low costand lowrecurrencerate.19However,althoughnumeroussurgical
methodshavebeendescribed,noneofthemencompassesall ofthesecharacteristics.20
Themaintechniquesused–incision and curettageand excision–resultinlargewounds,requiringlocalcareanda delayedhealing,aswellasthepossibilityoflocalrecurrence. Inanefforttominimizethisdrawback,varioustechniques havebeendescribed,e.g.,flaprotationandtheuseofflaps; however, these techniques are not without complications, andwoundinfection(0.8–7.6%),seroma(1.5–5.2%),dehiscence (4.1%),flapnecrosis(3%)andrecurrence(1.2–4.9%)havebeen reported.21–24
In 2013, Meinero et al. described a new technique for pilonidalcystapproachwiththeuseofafistuloscope.With this instrument and under direct vision, it is possible to destroyallgranulationtissueandtoremovetheentireinfected areaofthecyst,leavingasmallopenwoundfordrainage.In theirinitialseriesof11patients,allsubjectshadtheirwounds healedwithinonemonthaftersurgery,withanaveragereturn toworkin3.5days.
Therewasno recurrenceina6-monthfollow-up period (rangingfrom1to9months).12
In 2014, Milone et al. published their series with this procedure in 27 patients, with a 12-month follow-up. All woundshealedwithin15days,withrecurrenceinonlyone patient,twomonthsaftersurgery.Thesestudiesshowthat this isa very effectivetechnique forthe treatment ofthis disease.25
In this paper, we describe our experience with an initial case, using this technique in a 32-year-old male patient. The patient was placed in the prone position underspinalanesthesia and intravenoussedation.The fis-tula orifice was catheterized; then the fistuloscope was introduced, using a solution of glycine 1.5%. The tract of the cyst was identified and studied, with removal of hair inside the lesion. In sequence, the tract was cauterized, with removal of devitalized tissue; finally the drain ori-fice was enlarged. The patient has been followed up (to date,during10months),withgoodhealingandnosignsof recurrence.
Conclusion
Thisisaminimallyinvasiveprocedurewithlittleaggressionto thetissuesinvolved.Itsgreatadvantagesareanearlyreturnto activityandasmallsurgicalscar,withlesspain/inconvenience tothepatient.Ontheotherhand,thetechniquehasthe disad-vantageoftheavailabilityofafistuloscopekitforperforming theprocedure.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
r
e
f
e
r
e
n
c
e
s
1.BendewaldFP,CimaRR.Pilonidaldisease.ClinColonRectal Surg.2007;20:86–95.
2.BuczackiS,DrageM,WellsA,GuyR.Sacrococcygealpilonidal sinusdisease.ColorectalDis.2009;11:657.
3.BalsamoF,BorgesAMP,FormigaGJS.Cistopilonidal sacrococcígeo:resultadosdotratamentocirúrgicocom incisãoecuretagem.RevBrasColoproct.2009;29:325–8. 4.Ekc¸iB,Gökc¸eO.Anewflaptechniquetotreatpilonidalsinus.
TechColoproctol.2009;13:205–9.
5.SitM,AktasG,YilmazEE.Comparisonofthethreesurgical flaptechniquesinpilonidalsinussurgery.AmSurg. 2013;79:1263–8.
6.ParadesV,BouchardD,JanierM,BergerA.Pilonidalsinus disease.JViscSurg.2013;150:237–47.
7.MajeskiJ,StroudJ.Sacrococcygealpilonidaldisease.IntSurg. 2011;96:144–7.
8.MuziMG,MaglioR,MilitoG,NigroC,CiangolaI,BernagozziB, etal.Long-termresultsofpilonidalsinusdiseasewith modifiedprimaryclosure:newtechniqueon450patients.Am Surg.2014;80:484–8.
9.CorsiP,CorsiR,MouraL,GuerreiroT.Vasconcellos
Tratamentocirúrgicodocistopilonidalatravésderessecc¸ãoe fechamentoprimáriocomretalhocutâneo.RevBras
Coloproct.2004;24:203–7.
10.HorwoodJ,HanrattyD,ChandranP,BillingsP.Primary clousureorrhomboidexcisionandLimbergflapforthe managementofprimarysacrococcygealpilonidaldisease?A meta-analysisofrandomizedcontrolledtrials.ColorectalDis. 2012;14:143–51.
11.MahdyT.Surgicaltreatmentofthepilonidaldisease:primary closureorflapreconstructionafterexcision.DisColon Rectum.2008;51:1816–22.
12.MeneiroP,MoriL,GasloliG.Endosopicpilonidalsinus treatment(E.P.Si.T.).TechColoproctol.2014;8:389–92. 13.MendesCRS,FerreiraLSM,SapucaiaRA,LimaMA,Araujo
SEA.VAAFT–Videoassistedanalfistulatreatment:anew approachforanalfistula.JColoproctol.2014;34:62–4. 14.MendesCR,FerreiraLS,SapucaiaRA,LimaMA,AraujoSE.
Video-assistedanalfistulatreatment:technical
considerationsandpreliminaryresultsofthefirstBrazilian experience.ArqBrasCirDig.2014;27:77–81.
15.BlendewaldFP,CimaRR.Pilonidaldisease.ClinColonRectal Surg.2007;20:86–95.
16.BascomJ.Surgicaltreatmentofpilonidaldisease.BMJ. 2008;336:842–3.
17.MenzelT,DornerA,CramerJ.Excisionandopenwound treatmentofpilonidalsinus.Rateofrecurrenceandduration ofworkincapacity.DtschMedWochenschr.1997;122:1447–51. 18.VarnalidisI,LoannidisO,ParaskevasG,etal.Pilonidalsinus:a
comparativestudyoftreatmentmethods.JMedLife. 2014;7:27–30.
19.AkinciOF,CoskunA,UzunkoyA.Simpleandeffective surgicaltreatmentofpilonidalsinus:asymmetricexcision andprimaryclosureusingsuctiondrainandsubcuticular skinclosure.DisColonRectum.2000;43:701–6.
jcoloproctol(rioj).2015;35(1):72–75
75
21.DaphanC,TekeliogluMH,SayilganC.Limbergflaprepairfor pilonidalsinusdisease.DisColonRectum.2004;47:233–7. 22.Al-HassanHK,FrancisIM,NeglenP.Primaryclosureor
secondarygranulationafterexcisionofpilonidalsinus.Acta ChirScand.1990;156:695–9.
23.ErtanT,KocM,GocmenE,AslarAK,KeskekM,KilicM.Does techniquealterqualityoflifeafterpilonidalsinussurgery. AmJSurg.2005;190:388–92.
24.UrhanMK,KucukelF,TopgulK,OzerI,SariS.Rhomboid excisionandLimbergflapformanagingpilonidalsinus: resultsof102cases.DisColonRectum.2002;45:656–9. 25.MiloneM,MusellaM,SardoADS,BifulcoG,SalvatoreG,