w w w . r b o . o r g . b r
Original
article
Total
hip
arthroplasty
using
a
posterior
minimally
invasive
approach
–
results
after
six
years
夽
José
Ricardo
Negreiros
Vicente
∗,
Helder
Souza
Miyahara,
Carlos
Malheiros
Luzo,
Henrique
Melo
Gurgel,
Alberto
Tesconi
Croci
InstitutodeOrtopediaeTraumatologia,HospitaldasClínicas,FaculdadedeMedicina,UniversidadedeSãoPaulo,SãoPaulo,SP,Brazil
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received16October2013 Accepted20February2014 Availableonline31December2014
Keywords:
Hiposteoarthritis Hiparthroplasty
Minimallyinvasivesurgical procedures
a
b
s
t
r
a
c
t
Objective:Toevaluatethemedium-termclinical–functionalresults(minimumfollow-upof sixyears)fromtotaluncementedhiparthroplastyperformedbymeansofaposterior min-imallyinvasiveaccess,incomparisonwiththetraditionalrightlateralaccess.
Methods:Inacomparativeprospectivestudy,224adultpatientsunderwentelectivetotal hiparthroplastyduetoadiagnosisofprimaryorsecondaryosteoarthrosis.Agroupof103 patientswithposteriorminimallyinvasiveaccesswascomparedwithagroupof121patients withthetraditionalrightlateralaccess.Themeanlengthoffollow-upamongthepatients ofthissamplewas7.2years.Weevaluatedtheclinical–functionalandradiographicresults andoccurrencesofloosening,alongwithanycomplicationsthatoccurred,withaminimum follow-upofsixyears.
Results:Theclinical–functionalanalysesbeforethesurgicalprocedureandsixyears after-wardsweresimilarinthetwogroups(p=0.88andp=0.55).Onepatientintheminimally invasivegroupunderwentrevisionoftheacetabularcomponentandtwopatientsinthe con-trolgroupunderwentthesameprocedure(p=0.46).TheTrendelenburgclinicaltest,which showedweaknessofthehipabductormusculature,waspresentinfivepatientsoperated usingthetraditionallateralrouteandabsentinallthosewhounderwenttheminimally invasiveprocedure(p=0.06).Therewasnodifferenceregardingtheradiographicparameters obtained,eitherinacetabularorinfemoralpositioning(p=0.32andp=0.58).
Conclusions: Themedium-termclinicalandradiographicresultsandthecomplicationrates weresimilarbetweenthepatientswhounderwenttotalhiparthroplastybymeansofthe posteriorminimallyinvasiveaccessandthosewiththetraditionallateralaccess.
©2014SociedadeBrasileiradeOrtopediaeTraumatologia.PublishedbyElsevierEditora Ltda.Allrightsreserved.
夽
WorkdevelopedbytheHipGroupoftheInstituteofOrthopedicsandTraumatology,UniversityofSãoPauloMedicalSchool,SãoPaulo, SP,Brazil.
∗ Correspondingauthor.
E-mail:[email protected](J.R.N.Vicente). http://dx.doi.org/10.1016/j.rboe.2014.12.005
Artroplastia
total
do
quadril
feita
por
via
posterior
minimamente
invasiva
–
Resultados
após
seis
anos
Palavras-chave:
Osteoartritedoquadril Artroplastiadequadril Procedimentoscirúrgicos minimamenteinvasivos
r
e
s
u
m
o
Objetivo: Avaliaroresultadoclínico-funcionalemmédioprazo(seguimentomínimodeseis anos)daartroplastiatotaldoquadrilnãocimentadafeitaporacessominimamenteinvasivo (MIS)posteriorcomparadoaoacessolateraldireto(LD)tradicional.
Métodos: Emumestudocomparativoprospectivo,224pacientesadultosforamsubmetidos àartroplastiatotaldoquadrilemcarátereletivo,pordiagnósticodeosteoartroseprimária ousecundária,esecomparouogrupoMISposterior(103pacientes)comogrupoacessoLD tradicional(121).Amédiadetempodeseguimentodospacientesdaamostrafoi7,2anos. Avaliamososresultadosclínico-funcionaiseradiográficoseaocorrênciadesolturas,assim comocomplicac¸õesocorridascomumseguimentomínimodeseisanos.
Resultados: Aanáliseclínico-funcionalanteseseisanosapósoprocedimentocirúrgicofoi semelhantenosdoisgrupos(p=0,88ep=0,55).UmpacientedogrupoMISfoisubmetidoà revisãodocomponenteacetabularedoisdogrupocontroleforamsubmetidosaomesmo procedimento,p=0,46.OtesteclínicodeTrendelenburg,queevidenciouumafraquezada musculaturaabdutoradoquadril,estavapresenteemcincopacientesoperadospelavia lateraltradicionaleausenteemtodosossubmetidosaoMIS(p=0,06).Nãohouvediferenc¸a quantoaosparâmetrosradiográficosobtidostantodoposicionamentoacetabularquanto dofemoral(p=0,32,p=0,58).
Conclusões:Osresultadosemmédioprazo,clínicoseradiográficos,eataxadecomplicac¸ões foramsemelhantesentreospacientessubmetidosàartroplastiatotaldoquadrilpeloacesso posteriorminimamenteinvasivoepelavialateraltradicional.
©2014SociedadeBrasileiradeOrtopediaeTraumatologia.PublicadoporElsevier EditoraLtda.Todososdireitosreservados.
Introduction
Totalhip arthroplasty performedby means ofaminimally
invasive accessemerged because ofthe trend observed in
other fields of surgery. It had the aims of ensuring better results,fewercomplications,lessperioperativemorbidityand alowercostburdenforpublicandprivatehealthcareservice providers.1,2
Several studies have shown that a minimally invasive
accesscanleadtobetterrecoveryintheimmediate postop-erativeperiod,withlesspain,lessbleedingduringthehospital stay,less muscleinjuryand,consequently,shorterhospital stay.3–5
However, in comparing traditional and minimally
inva-sive surgical accesses, other authors have shown similar
short-termresults,withoutanyrealbenefit.6,7Someauthors
have even warned of higher complication rates and risks
with some minimally invasive accesses, such as a single
anterior access, and have reported unusual complications
andprolongeddurationofsurgery,alongwithlonglearning curves.8,9
Our objective here was toassess the clinical and
func-tionalresultsoverthemediumterm(minimumfollow-upof
sixyears)andthecomplicationsfromuncementedtotalhip
arthroplasty performedby means ofaposterior minimally
invasiveaccess,incomparisonwithatraditionalrightlateral access.
Material
and
methods
Afterobtainingapprovalfromourinstitution’sresearchethics
committee,aprospectivecomparativestudywasconducted
in which 224 adult patients underwent elective total hip
arthroplasty due to a diagnosis of primary or secondary
osteoarthrosis.Thepatientswereselectedfromthewaiting listofourhospital’sHipGroup.
ThesamplesaredescribedinTable1.
Randomizationwasperformedbymeansofasequenceof
randomnumbers,withdivisionintotwogroupsatthetime
ofmakingthesurgicalappointments.Thiswasdonebya sur-geonwhowasnotdirectlyinvolvedinthisstudy,withoutthe knowledgeofthesurgeonwhowasthefirstauthor.Inthefirst group,theposterioraccessfirstdescribedbyMoorewasused, withsmall-sizedincisionsandminimaldissectionofsoft tis-sues.Inthepatientsofthecontrolgroup,thetraditionalright
Table1–Sampleparameter.
Minimally invasivegroup
Controlgroup pvalue
lateralaccessroutefirstdescribedbyHardingerwasused,but withthepatientinlateraldecubitus.Therewere103patients intheminimallyinvasiveaccessgroupand121intheright lateralaccessgroup.
Themeanlengthoffollow-upforthewholesamplewas7.2 years,witharangefrom6.1to9years.
Thecriteriafornon-inclusioncomprisedpresentationof anytypeofcoagulopathy,systemicarterialhypertensionthat wasnotunderpharmacologicalcontrol,previoushipsurgery orsequelaefromcongenitalhipdysplasiaofCrowetypes2,3 or4thatrequiredstructuralgraftingintheacetabularroof.
Theexclusion criterion was loss offollow-up occurring beforethetimeoftheoutpatientassessmentinthesixthyear aftertheoperation.
Allthepatientsfollowedthesameprotocolfor postopera-tiveanalgesia,whichconsistedof100mgoftramadol(Pfizer®)
intravenously every eight hours and 100mg of ketoprofen
(Eurofarma®)inasingleintravenousdosedailyuntilthedayof
hospitaldischarge.Thromboembolicprophylaxiswas admin-isteredtoallthepatients,consistingof40mgofenoxaparin appliedsubcutaneously(Sanofi-Aventis®),startingonthefirst
dayaftertheoperationandcontinuinguntilthe30thday. All the patients were discharged on the fifth day after theoperationandweregivenguidanceregarding physiother-apyandanticoagulantandanalgesicmedications(500mgof paracetamolorallyeverysixhours,ifnecessary).
Inthisstudy,weusedtwomodelsofuncemented prosthe-sis(MeridianfemoralnailwithVitalock-Stryker®acetabulum
and Bicontact femoral nail with Aesculap® Plasmacup®
acetabulum). The choice between these two implants was
basedmerelyontheiravailabilityonthe dayonwhichthe patientwasoperated.Bothofthesemanufacturerswere sup-plierstoourhipsurgeryserviceatthetimeofthisstudy.
All the patients inthe minimally invasive accessgroup wereoperatedbythefirstauthorofthisstudyandthepatients intherightlateralaccessgroupwereoperatedbythree sur-geons,amongwhomwasthefirstauthor.
Somepointsrelatingtothe posteriorminimallyinvasive accessneedtobehighlighted.Thisisanaccessroutethat impliesagentle learningcurve,evenforsurgeonswho are accustomedto thetraditional posterioraccess. The princi-pleofthemovingwindowmaybeofgreatvaluewithregard toacetabularand femoralaccess:the positionofthe spac-ersshouldbechangedaccordingtotheregiontobeprepared, withsoft-tissuedisplacementdistallyforpreparationofthe acetabulumandproximallyforpreparationofthefemur,soas toavoidgreattensioningofthesurfacetissuesandminimize theriskofscarcomplicationsatthesurgicalincision.
The physiotherapy protocol used consisted of assisted
activeflexionoftheanklesandkneesusinganabductionpad, startingonthefirstpostoperativeday;andgaittrainingwith partialweight-bearingstartingonthesecond day,withfull loadappliedsixweeksaftertheoperation.Eachpatient’s evo-lutionwasfollowedupbymeansofreturnvisitsscheduledto takeplaceone,three,six,12and24weeksaftertheoperation. Thereturnvisitsbecameannualafterthefirstpostoperative year.
A clinical–functional assessment was made and the
radiographic criteria were also analyzed in both groups.
Fortheclinical–functionalassessment,theHarrisHipScore
questionnairewasusedbeforetheoperation(duringtheweek precedingthesurgery),sixmonthsandoneyearafterwards and,finally,sixyearsafterthesurgery.Sixyearsoffollow-up
was consideredtobethe minimumlengthoftime forthis
criterioninthepresentstudy.
Possiblelate complicationsand asepticloosening ofthe prostheticcomponentsamongthepatientsofthisstudywere evaluatedaftersixyearsoffollow-up.
Aradiographicassessmentwasmadeatthereturnvisitsix monthsaftertheoperation.Theacetabularpositioningwas consideredtobegoodiftheabductionangleofthe acetabu-lumwasbetween35◦ and50◦.Thefemoralpositioningwas
consideredtobegoodifthefemoralcomponentspresented
between0◦and5◦ofvalgus.
PresenceorabsenceoftheTrendelenburgclinicalsignwas measuredatthereturnvisitsixyearsaftertheoperation.
Thelinearradiographicwearpresentedbythepolyethylene wasmeasuredusingacompassandrulermarkedin millime-tersatthesixth-yearfollow-up.Thevariationinthicknessof
thepolyethylenebetweentheupperandlowerportionswas
evaluatedbasedonthesphericityoftheprosthetichead.We consideredthatthewearwasunacceptableifitwas≥1mm,
whichwouldrepresentmorethan0.1mmoflinearwearper
year, given the length of follow-up of the patients in our study.10
Quantitative variables with Gaussian distribution were comparedusingthenon-pairedStudentttest.Datathatdid notpresentnormaldistributionwereevaluatedbymeansof
nonparametric tests.Comparisonsbetweenthe twogroups
were madeusingtheMann–Whitneytest.Qualitative
(non-numerical)datawereanalyzedusingthechi-squaretest,or theFishertestwhennecessary.Thelevelofstatistical signifi-cancewassetatp=0.05.
Results
Regardingtheprosthesismodelsused,theMeridian/Vitalock (Stryker®)implantwasmoreprevalentinbothgroupsthanthe
Bicontact/Plasmacup(Aesculap®),butwithoutanysignificant
difference(60.2%versus53.7%;p=0.34).
Adiagnosisofprimaryhiposteoarthrosiswasmadein61 patientsoftherightlateralgroup(50.4%)and57ofthe mini-mallyinvasivegroup(55.3%),withp=0.5.Alltheotherpatients werediagnosedwithosteoarthrosissecondarytoother patho-logicalconditions,whichincludedosteonecrosis,seronegative
arthritis, sequelae from Pèrthes disease, sequelae from a
slipped epiphysis, rheumatoid arthritis and post-traumatic hiparthritis.
Thelinearradiographicwearofthepolyethylenewas mea-suredusingacompassandrulermarkedinmillimetersatthe sixth-yearfollow-up.Agreaterdegreeofwearthanexpected (>1mm)wasobservedin30%ofthepatientsintheminimally invasivegroup,versus33.8%ofthecontrols,withp=0.56.
Intheminimallyinvasivegroup,noacetabularorfemoral osteolysiswasidentifiedinanyofthepatientsfromthesixth
year onwards. However,osteolysis was diagnosed in three
In relation to the acetabular and femoral positioning amongthepatientswithaminimallyinvasiveaccess,
unsa-tisfactory results were noted in 5.8% of the acetabular
components and in4.8%of the femoralnails.In
compari-son,inthe controlgroup,therewere unsatisfactoryresults in9.9%oftheacetabularcomponentsand7.4%ofthefemoral components,withpvaluesof0.32and0.58,respectively.
TheTrendelenburg clinical test, which shows weakness
oftheabductormusculatureofthehip,waspositiveinfive patientswhowereoperatedbymeansofthetraditionallateral
approachbut wasabsentfrom all thepatients who
under-wentsurgerybymeansoftheposteriorminimally invasive
access,althoughtherewasnostatisticallysignificant differ-ence(p=0.06).
The clinical–functional assessments in the two groups
beforethesurgeryweresimilar(meanof47.5intheminimally invasivegroupand48inthecontrolgroup)(p=0.88).
TheHarrisHipScoreaftertheoperationshowedthatthere hadbeenanimprovementinbothgroups,withsimilarmean scores(86intherightlateralgroupversus87.6inthe mini-mallyinvasivegroup;p=0.55).
Asepticacetabularlooseningoccurredinonepatient,who hadbeenoperatedbymeansoftheminimallyinvasive pos-terioraccess.Thiscaseunderwentrevision12monthsafter theinitialsurgery.Revisionoftheprosthesiswasnecessary intwoofthepatientsinthecontrolgroup:thepolyethylene inonepatientwasexchangedafter6.5yearsoffollow-upand acetabularrevisionwasperformedinanotherpatientofthis groupaftersevenyears(p=0.46).
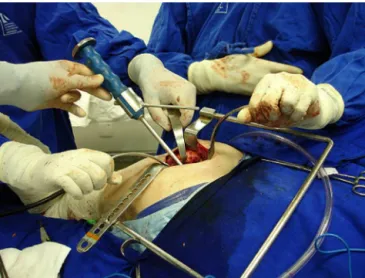
Theonlystatisticallysignificantresultwasthesizeofthe incision(p<0.001),withameanof95.1mmfortheminimally invasiveaccessand169.8mmforthetraditionallateralaccess (Fig.1).
Regarding complications, there were two cases in the
minimallyinvasivegroup:oneofmedialacetabular fractur-ingwithoutdisplacement,whichwastreatedconservatively; andoneofheterotopicossification,whichrequiredsurgical resection.Inthecontrolgroup,thereweretwocasesoffemoral fractures,whichweretreatedbymeansofcerclageduringthe samesurgicalprocedure;onecaseofdislocation,whichwas treatedbymeansofclosedreduction,withoutrecurrence;one caseofsuperficialinfection,whichwastreatedbymeansof oralantibiotictherapy; andone caseofneuropraxiaofthe ulnarnervecausedbythepositioningonthesurgicaltable, whichregressedaftereightweeks.Nosignificantdifference wasobservedbetweenthegroups(p=0.45).
Discussion
Inourstudy,wenotedthatthemeanageofourpatientswas lower than seen instudies in the literature,which mostly showedmean ages greater than 60years.2,11 This can
per-hapsbeexplainedbytheconsiderablenumbers ofcasesof
osteoarthrosis secondary to systemic and rheumatological
diseasesthatwereobservedinoursetting(almosthalfofour patients).Anotherpossiblecauseforthisfindingwasperhaps thetypicalpyramidalagedistributionoftheBrazilian popula-tion,whichdiffersfromthatofEuropeanorNorthAmerican
countries. Thislower mean age may representa sourceof
Fig.1–Scarof5.5cmsixmonthsaftertheoperation.
bias,bothtowardbetterrecoveryfromtheacute postopera-tivephaseandtowardthecomplicationsinherenttowearand looseningofthearthroplasty,giventhatthesepatients theo-reticallyhaveahigherdegreeofphysicalandworkactivity.
Otherpossiblesourcesofbiasintheresultsobtainedinthe presentstudyincludethefactthattwoprosthesismodelswere usedinbothgroups,althoughbothmodelswereuncemented. However,mostofthestudieswithlargesampleshavetended topresent thissame bias.Regardingthe controlgroup,the factthattheprocedureswereperformedbydifferentsurgeons mightalsobeconsideredtobeasourceofbias,although diver-sityofsurgeonshasalsobeenreportedbyagoodproportion ofpreviousauthors.
Theuseofprostheseswithatribologicalpairconsistingof aconventionalpolyethyleneinsertandametalhead,together withthepatients’lowerageandconsequentlyhigherlevelof activity,mayhavebeenresponsibleforthelinearweargreater thanexpectedthatwasfoundinone-thirdofthecases,and for theearly acetabularosteolysisthat was foundinthree patientsofthecontrolgroup.However,weemphasizethatthe methodologyusedformeasuringthewearofthepolyethylene presentsamarginoferrorofaround15%.Methodsofgreater precisionsuchascomputerizedthree-dimensionalmodelsare usedtoday,butthesewerenottakenintoconsiderationinthe
present studybecausetheydidnotformtheauthors’main
objective.
Fig.2–Straightacetabularimpactor,whichmightmakeit difficulttopositionthecomponent.
(>52)tendtopresentgreatertechnicaldifficultyforsurgeons, withahigherriskoflateralizationandgreaterabductionangle fortheacetabularcomponent.Thisresultsfromtheangleof attackoftheacetabularreamer,whichisharmfulparticularly
whenreamers and impactors that are adaptedforsmaller
accessesarenotused(Fig.2).12
Weaknessoftheabductormusculature,asrepresentedbya positiveTrendelenburgtest,wasonlyfoundinpatientsinthe groupoperatedbymeansofalateralaccess.Thisresultwas notsignificant(p=0.06).Kinematicgaitstudieshaveproven thatbetterresultsare obtainedwhentheaccessuseddoes notinterferedirectlywiththeintegrityofthismusculature.13
Most studies have shown that the acute postoperative
recoveryisbetterwhenaminimallyinvasiveaccessisused, withlessbleeding,lowermuscledamageandshorter hospi-talstay.Thequestionofbleedingduringthehospitalstayis anotherpolemicalpointbecausealthoughmostauthorshave reportedmeanvolumesofbleedingof500mL,2,3,14,15the inci-denceoftransfusionsamongthepatientsiscloseto50%.This denotesa contradictionand a likelyunderestimate, which
has been confirmed by other studies in which the central
scopewasbloodvolumelossandthemethodologywasmore
detailedforsuchestimates.5,16,17
Our study, with a follow-up of more than six years,
presented results similar to data in the literature on this
topic, as demonstrated in a recent meta-analysis, which
showed similar evolution inthe two groups, both in rela-tion to the radiographicparameters and in relation tothe clinical–functionalscore ofthe Harris HipScore, atall the timesevaluated.However,themediumandlong-term follow-upseemstobeuncertainandinconclusive,giventhescarcity ofcomparativestudieswithlongerfollow-ups,andthereisno evidencesofarregardingthesuperiorityoftheseaccessesin relationtothetraditionalroutes.18
Overall,inthewholesample,weonlyobservedonecaseof dislocation.Webelievethatthislowincidencewasduetothe intensiveworkconductedbythephysiotherapyteamofour service,inwhichposturaleducationalmeasureswere imple-mentedtodiminishtheriskofthiscomplication.Moreover,in
ourstudy,wewereonlydealingwithpatientswithadiagnosis ofosteoarthrosis.Itiswellknownthatthesepatientspresent lowerriskthandopatientswithadiagnosisoffracturingof thefemoralneckwhoundergototalhiparthroplasty.
Wechosetoevaluateoveralloccurrencesofcomplications pergroup,inacomparativemanner,becausethesamplesize wouldbeinsufficientforustoevaluateeachcomparisonin detailaccordingtoeachtypeofcomplicationthatoccurred.
Theonlyvariableevaluated inthis study thatshoweda significant differencefortheminimally invasiveaccess,i.e. thesmaller-sizedincision,theoreticallywouldindicate that the estheticresultwouldbe better.However,in2005, Mow etal.19demonstratedworsescarringresultsfromsmall inci-sions.Inoursample,therewerenoestheticcomplaints,but itneedstobeborneinmindthatthisshouldbelastcriterion forindicatingalessinvasiveaccess.
Conclusion
Themedium-termclinicalandradiographicresultsandthe
complication rate are similar forpatients undergoing total hiparthroplastybymeansofaposteriorminimallyinvasive access and by means of the traditionalright lateral route.
However, the right lateral access more frequently causes
insufficiencyoftheabductormusculature,inrelationtothe posteriorminimallyinvasiveaccess.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
r
e
f
e
r
e
n
c
e
s
1.WenzJF,GurkanI,JibodhSR.Mini-incisiontotalhip arthroplasty:acomparativeassessmentofperioperative outcomes.Orthopedics.2002;25(10):1031–43.
2.GoldsteinWM,BransonJJ,BerlandKA,GordonAC.
Minimal-incisiontotalhiparthroplasty.JBoneJointSurgAm. 2003;85Suppl.4:33–8.
3.MattaJM,ShahrdarC,FergusonT.Single-incisionanterior approachfortotalhiparthroplastyonanorthopaedictable. ClinOrthopRelatRes.2005;441:115–24.
4.BergerRA.Totalhiparthroplastyusingtheminimally invasivetwo-incisionapproach.ClinOrthopRelatRes. 2003;(417):232–41.
5.VicenteJR,CrociAT,CamargoOP.Bloodlossintheminimally invasiveposteriorapproachtototalhiparthroplasty:a comparativestudy.Clinics.2008;63(3):351–6[SaoPaulo]. 6.DeBeerJ,PetruccelliD,ZalzalP,WinemakerMJ.
Single-incision,minimallyinvasivetotalhiparthroplasty: lengthdoesn’tmatter.JArthroplasty.2004;19(8):945–50. 7.OgondaL,WilsonR,ArchboldP,LawlorM,HumphreysP,
O’BrienS,etal.Minimal-incisiontechniqueintotalhip arthroplastydoesnotimproveearlypostoperativeoutcomes. Aprospective,randomized,controlledtrial.JBoneJointSurg Am.2005;87(4):701–10.
9. BalBS,HaltomD,AletoT,BarretM.Earlycomplicationsof primarytotalhipreplacementperformedwithatwo-incision minimallyinvasivetechnique.JBoneJointSurgAm.
2005;87(11):2432–8.
10.GriffithMJ,SeidensteinMK,WilliamsD,CharnleyJ.Socket wearinlowfrictionarthroplastyofthehip.ClinOrthopRelat Res.1978;(137):37–47.
11.SwansonTV.Earlyresultsof1000consecutive,posterior, single-incisionminimallyinvasivesurgerytotalhip arthroplasties.JArthroplasty.2005;20(Suppl3):26–32. 12.VicenteJR,CrociAT,CamargoOP.Restaurac¸ãodocentrode
rotac¸ãonaartroplastiatotaldoquadrilminimamente invasiva.ActaOrtopBras.2009;17(2):14–7.
13.RitterMA,HartyLD,KeatingME,FarisPM,MedingJB.A clinicalcomparisonoftheanterolateralandposterolateral approachestothehip.ClinOrthopRelatRes.2001;(385):95–9. 14.ChimentoGF,PavoneV,SharrockN,KahnB,CahillJ,Sculco
TP.Minimallyinvasivetotalhiparthroplasty.Aprospective randomizedstudy.JArthroplasty.2005;20(2):139–44.
15.WrightJM,CrockettHC,DelgadoS,LymanS,MadsenM, SculcoTP.Mini-incisionfortotalhiparthroplasty.A prospective,controlledinvestigationwith5-yearfollow-up evaluation.JArthroplasty.2004;19(5):538–45.
16.RosencherN,KerkkampHEM,MacherasG,MunueraLM, MenichellaG,BartonDM,etal.Orthopedicsurgery
transfusionhemoglobinEuropeanoverview(OSTHEO)study: bloodmanagementinelectivekneeandhiparthroplastyin Europe.Transfusion.2003;43(4):459–69[Paris].
17.PiersonJL,HannonTJ,EarlesDR.Ablood-conservation algorithmtoreducebloodtransfusionaftertotalhipand kneearthroplasty.JBoneJointSurgAm.2004;86(7):1512–8. 18.MoskalJT,CappsSG.Islimitedincisionbetterthanstandard
totalhiparthroplasty?Ameta-analysis.ClinOrthopRelat Res.2013;471(4):1283–94.
19.MowCS,WoolsonST,NgarmukosS,ParkEH,LorenzPH. Comparisonofscarsfromtotalhipreplacementsdonewitha standardoramini-incision.ClinOrthopRelatRes.