w w w . j c o l . o r g . b r
Journal
of
Coloproctology
Technical
Note
Resection
of
ischiorectal
fossa
tumors
–
surgical
technique
Eduardo
Fonseca
Alves
Filho
a,∗,
Alexandre
Lopes
de
Carvalho
a,
Paulo
Frederico
de
Oliveira
Costa
a,
Antonio
Carlos
de
Carvalho
b aHospitalPortuguêsdaBahia,Salvador,BA,BrazilbHospitalGeralRobertoSantos,Salvador,BA,Brazil
a
r
t
i
c
l
e
i
n
f
o
Articlehistory:
Received3April2015
Accepted13April2016
Availableonline9May2016
Keywords:
Ischiorectalfossatumors
Neoplasms
Solitaryfibroustumors
a
b
s
t
r
a
c
t
Primarytumorsoftheischiorectalfossaarerare,theycanbecongenital,acquiredor
neo-plastic.Accuratediagnosisoftencannotbedonepreoperativelyandimagingstudiessuchas
computedtomographyandespeciallymagneticresonanceimagingcandefinethesizeand
anatomicalrelationshipsofthelesions.Surgicaltreatmentischallengingbecauseof
diffi-cultaccessoftheregionwhichispreferablyperformedbyposteriorapproach.Wedescribe
theetiology,diagnosisandoperativetechniqueoftumorsoftheischiorectalfossa.
©2016SociedadeBrasileiradeColoproctologia.PublishedbyElsevierEditoraLtda.This
isanopenaccessarticleundertheCCBY-NC-NDlicense(http://creativecommons.org/
licenses/by-nc-nd/4.0/).
Ressecc¸ão
de
tumores
da
fossa
isquiorretal
–
técnica
cirúrgica
Palavras-chave:
Tumoresdafossaisquiorretal
Neoplasias
Tumoresfibrosossolitários
r
e
s
u
m
o
Tumoresprimáriosdafossaisquiorretalsãoraros,epodemsercongênitos,adquiridos,ou
neoplásicos.Comfrequêncianãoépossíveloestabelecimentodeumdiagnósticopreciso
nopré-operatório,eestudosimaginológicos,comoatomografiacomputadorizadae,em
especial,asimagensporressonânciamagnética,podemdefinirasdimensõeserelac¸ões
anatômicasdaslesões.Otratamentocirúrgicoétarefadesafiadora,emdecorrênciadodifícil
acessoàregião,que,depreferência,sefazporumaabordagemposterior.Descrevemosa
etiologia,diagnósticoetécnicaoperatóriadetumoresdafossaisquiorretal.
©2016SociedadeBrasileiradeColoproctologia.PublicadoporElsevierEditoraLtda.Este
´eumartigoOpenAccesssobumalicenc¸aCCBY-NC-ND(http://creativecommons.org/
licenses/by-nc-nd/4.0/).
∗ Correspondingauthor.
E-mails:[email protected],[email protected](E.F.A.Filho).
http://dx.doi.org/10.1016/j.jcol.2016.04.006
2237-9363/©2016SociedadeBrasileiradeColoproctologia.PublishedbyElsevierEditoraLtda.ThisisanopenaccessarticleundertheCC
anorectalregion(Fig.1),ithasapyramidalshapeand both
communicateposteriorlythroughthepostanaldeepspace,
betweenthelevatoraniandtheanococcygeusligament.The
IRFrelatesmediallywiththerectum,thelevatoraniandthe
externalanal sphincter and anteriorlywith the superficial
anddeeptransverseperinealmuscle.Theobturatorinternus
definethelateralmargin;theIRFisboundedinferiorlybythe
perineal skin. Craniallythe levator aniseparate IRF ofthe
suprelevatorspace.TheIRFcontainsadiposetissue,nerves,
vesselsandlymphfromthevesselsandthepudendalnerves.1
Tumorsinthisregionarepresentedasaperineal,gluteal
(Fig.2),orlabialmass.Largelesionsthatcompressthe
rec-tum and uro-genital organs can cause symptoms such as
Fig.1–Anatomyoftheischiorectalfossa.
R,rectum;IRF,ischiorectalfossa;AE,analesphincter;LA, levatoranimuscle;OI,obturatorinternusmuscle;IT,ischial tuberosity.
Fig.2–Bulgingleftbuttock.
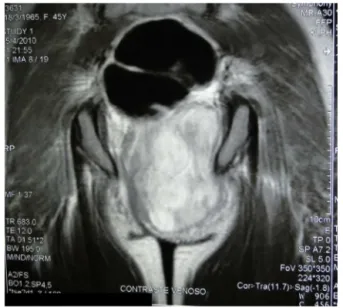
Fig.3–MRIofthepelvisshowingalargemassinIRF, compressingtherectum,vaginaandthelevatorani.
constipation,dispaurenia,dysuriaandperinealpain.3
Infec-tion, rupture and malignant transformation can occur as
complications.3,4
Primary tumorsoftheIRF are rare. Theclinical
diagno-siscannotbedonealonebecauseofthedepthofthelesions.
Imagingexams,particularlyMRIcandeterminethepresence
ofexpansivelesionsintheregionanditsanatomical
relation-ships,butthediagnosiscanonlybedonewithpercutaneous
needlebiopsies,incisionalorexcisionalbiopsy.Results
neg-ativeformalignancybyneedleorincisionalbiopsydoesnot
ruleoutthepossibilityofmalignancy.MRI(Fig.3)issuperior
toCT(Fig.4)becauseithasbetterresolutionwithcontrast
infusion.1
TheresectionoftumorsoftheIRFisparticularly
challeng-ingbecauseofthedifficultyinaccessingthroughananterior
approach.Aposteriorapproachcombinedornotwithan
ante-rioraccessisused.Partofthesacrummayhavetoberemoved,
especiallyifthetumorislargeandextendtotheotherIRF.2
Amputationoftherectumisrequiredwhenthereisinvasion
oftherectum.2
Fig.5–Dissectionfromthesubcutaneoustissuetothe leveloftheglutealmuscles.
ThehistologicaldiagnosisoftumorsoftheIRFdependson
theirembryologicalorigin.Theycanbecongenital,acquired
orneoplastic.
Thepurposeofthisstudydescribesthesurgicaltechnique
ofresectionsoftumorsoftheIRFandtheiretiology.
Material
Operativetechnique:“jack knife”prone position, stretchof
buttocks:(1)verticalpara-sacralincisionanddissectionfrom
thesubcutaneoustissuetotheleveloftheglutealmuscles
(Fig.5);(2)identificationofthebottomedgeofthetumorand
theischialtuberosity,sectionofthesacrotuberousligament
andreleaseofthetumorfromthegluteusmaximus(Fig.6)or
itsresectionifthereisinvasionofthemuscle;(3)ifnecessary
thelowerpartofsacrumcanberesectedbutonlybelowS3
leveltopreservetherootofpudendalnerve;(4)medialand
cranialdissectionwithreleaseoftherectum(Fig.7),theanal
sphincterandthelevatoranifromthetumor;(5)closingthe
woundbyplansanddrainageoftheregionwithsuctordrain
(Fig.8).
Fig.6–Releaseofthetumorfromgluteusmaximus.
Fig.7–Releaseoftherectum.
Discussion
Congenitaltumors
Gardner’sduct cysts arecommon invagina,resultingfrom
incomplete regression of Wolffian ducts. Large cysts can
extendtotheIRF.Histologicallytheyhavecoatedorcuboidal
columnarepithelium.OnMRIthe lesionshowshigh signal
intensityandCTattenuationofasignalsimilartowater.1
Giantepidermalcystischaracterizedfromtheradiological
pointofviewbyhomogeneous,unilocularcysticlesion,well
demarcated,histologicallyarecomposedofkeratinsquamous
epithelialcells.ThecharacteristicsofthecystsonMRIare
sim-ilartoepidermalcystsofGardner’sduct.Ithasnomalignant
potentialdescribed.1,3
Tailgutcystisanhamartoma,duetotheincomplete
regres-sionofembryonicstructuresoftheanus.Itusuallyoccursin
theretro-rectalspacebutcanextendtotheIRF.Usuallythere
isahistoryofdiagnosisandtreatmentofanorectalabscesses
and fistulas. CT scan shows a well-defined solid or liquid
massintheretro-rectalspace,withoutinvasionofadjacent
structures.Differentialdiagnosisismadewithchordomas,
ter-atomas,rectal duplicationandmeningomyelocele. Thereis
potentialformalignancy.1
toneum, pelvis, presacral region and liver.4 There is little
literature on the SFT and only one report of involvement
of the IRF.2 Case reports of SFT in other regions, which
followedpatients forupto41 monthsshowedless
aggres-sivebehavior, evenwhen thereare histologicalfeatures of
malignancy (EMA, S 100 protein, desmin, epithelial
mem-braneantigenandneurofilament)showednorecurrencesor
metastasis.3,4 The importanceof recognizingthese tumors
shouldbeinitsdifferentiationfrommoreaggressivetumorsas
liposarcoma.4
LipomasonCTappearaslesionswithsignalsimilarto
sub-cutaneoustissue.Largeseptatedtumorsareindistinguishable
fromlow-gradeliposarcomas.1
Aggressiveangiomyxomaoccursmostcommonlyinyoung
women,affectingsofttissuessuchasthepelvis,perineum,
buttocks,vulva,retroperitoneum andinguinal regions,
sec-ondaryinvolvementoftheIRFiscommon.OnCTthereisa
hypoorisoattenuatingsign.1Theyhaveagelatinous
appear-anceandarelocallyinvasive.5
Malignant peripheral nerve sheath often exhibits areas
of benign appearance indistinguishable from fibromatosis.
Onefeatureisthatsuchtumorscanalsobefocal,
explain-ingtheoriginaldiagnosiserrors.Theyarehighlyaggressive
and difficult to handle. Systemic spread is often the
ulti-mate cause of death, although inoperable disease is also
common.6
Trichilemmal proliferative tumor (TPT) is a tumor that
develops from the outer sheath cells or follicular usually
aftertrauma orinflammation. Thistumorhas aslow
evo-lution and occurs in 90% of the time on the scalp, more
rarely other sites have been reported (trunk, face, pubic
area, vulva, members...). They can be large and
malig-nant transformation is rare.7 The immuno-histochemical
study isanaid todiagnosis ofmalignancyofTPTand the
differentialdiagnosismustbedonewithsquamouscell
car-cinoma.CD34,amarkerofdifferentiationofhairisweakly
positive in malignant TPT and negative in squamous cell
carcinoma.
Plexiformneurofibroma ispathognomonic ofVon
Reck-linghausen syndrome, characterized by diffuse growth of
Schwann cells along the nerves affected first. It is most
commonly seen in the extremities, mediastinum, neck
and pelvis. Involvement of the pudendal nerve can occur
withmultiplemassesofvariable sizewithlowattenuation
atCT.
Malignant histiciotoma can also occur in the IRF and
depend on location can be accessed by other routes of
surface.
OtherIRFmasses
Abscesses are associated with signs of inflammation and
generally arise from adjacent inflammatoryand infectious
processes,especiallyfromanorectaldiseases.InCTandMRI
appearsas fluidcollections withenhancement ofthe
cap-sule in contrast phase. Other signs include cellulitis and
edemacharacterizedbyincreasedattenuationof
ischiorec-talfat,gasandobliterationofadjacenttissues.Hematomas
are caused by localtrauma, acute lesions show up on CT
as hyper attenuating lesions with fluid levels and chronic
lesions with low attenuation and can be mistaken for
abscesses.1
Conclusion
NeoplasmsoccurringintheIRFmustbetreatedtakinginto
accounttheanatomyoftheregion. Thepreferablerouteof
accessisposterior,andmayrequirepartialresectionofthe
sacrum.Thedefinitivediagnosiscanonlyhappenwith
com-pleteresectionofthetumoranditssubsequentpathological
study
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
r
e
f
e
r
e
n
c
e
s
1.LlaugerJ,PalmerJ,PérezC,MonillJ,RibéJ,MorenoA.Normal andpathologicischiorectalfossaatCTandMRimaging. Radiographics.1998;18:61–82.
2.MillerM,KulaylatMN,FerrarioT,KarakousisCP.Resectionof tumorsoftheischiorectalfossa.JAmCollSurg.
2003;196:328–32.
3.NgSSM,HonSSF,WongJHM,LeeJFY.Radiologyforthe surgeon.Soft-tissuecase59.CanJSurg.2006;49:435–6.
4.YapT,HamzahL,OshowoA,TaylorI.Myxoidsolitaryfibrous tumouroftheischiorectalfossa.EurJSurgOncol.
2003;29:98–100.
5.SatheshkumarT,SaklaniAP,BanerjeeD,JonesDR. Angiomyofibrosarcoma:arareischiorectalfossaswelling. HospMed.2003;64:244–5.
7. MakhloufZ,VerolaO,SenejouxA,DuvalA,TerrisB,Balaton A,etal.Tumeurtrichilemmaleproliferantedelarégion ischio-rectale.AnnPathol.2011;31:316–9.
8. SteverMR,HernandezE,SakasEL.Malignantfibrous histiocytomaofthepelvis.GynecolOncol.1988;30: 285–90.
9.LimaMA,PozzobonBHZ,FonsecaMFM,HortaSHC,Formiga GJS.LeiomiossarcomaPerineal:RelatodeCasoeRevisãoda Literatura.RevBrasColoproct.2010;30:352–5.