REVISTA
BRASILEIRA
DE
ANESTESIOLOGIA
OfficialPublicationoftheBrazilianSocietyofAnesthesiologywww.sba.com.br
SCIENTIFIC
ARTICLE
Subarachnoid
clonidine
and
trauma
response
in
cardiac
surgery
with
cardiopulmonary
bypass
夽
Claudia
Gissi
da
Rocha
Ferreira
∗,
Sérgio
Bernardo
Tenório
HospitaldeClínicas,UniversidadeFederaldoParaná(UFPR),Curitiba,PR,Brazil
Received1December2012;accepted9April2013 Availableonline31March2014
KEYWORDS
Clonidine; Traumaticstress; Cardiacsurgery
Abstract
Backgroundandobjectives: Theintensetraumaresponsetriggeredbycardiopulmonarybypass canleadtoincreasedmorbidityandmortality.Thepresentstudyevaluatedwhetherclonidine, adrugoftheclassof␣-2agonists,administeredbyspinalroute,withoutassociationwithlocal anestheticsoropioids,reducesthisresponseincardiacsurgerywithcardiopulmonarybypass.
Method: Atotalof27patientsbetween18and75yearsold,dividedbynon-blindedfashioninto acontrolgroup(15)andaclonidinegroup(12),werestudied.Allpatientsunderwentidentical techniqueofgeneralanesthesia.Then,onlytheclonidinegroupreceived1gkg−1clonidineby spinalroute.Levelsofbloodglucose,lactateandcortisolweremeasuredatthreeconsecutive times:T1,atthetimeofinstallationofinvasive arterialpressure;T2,10minafterthefirst doseforcardioplegia;andT3,atthetimeofskinsuture;andtroponinIvaluesatT1andT3. ThevariationofresultsbetweenT2---T1,T3---T2,andT3---T1wasalsoevaluated.
Results:Therewas astatisticallysignificantdifferenceonlywithrespect tothevariationin bloodglucoseintheclonidinegroup:T3---T2,p=0.027andT3---T1,p=0.047.
Conclusions: Spinalclonidineatadoseof1gkg−1didnotdecreasebloodmeasurementsof troponin, cortisol,orlactate.Bloodglucose suffered amoremoderatevariationduringthe procedureintheclonidinegroup.Thisfact,alreadyreportedintheliterature,requiresfurther investigationtobeclarified.
© 2014SociedadeBrasileirade Anestesiologia.Publishedby ElsevierEditoraLtda.Allrights reserved.
PALAVRAS-CHAVE
Clonidina;
Estressetraumático; Cirurgiacardíaca
Clonidinasubaracnóideaerespostaaotraumaemcirurgiascardíacascomcirculac¸ão extracorpórea
Resumo
Justificativaeobjetivos: Aintensarespostaaotraumadesencadeadapelacirculac¸ão extracor-póreapodeconduziraoaumentodamorbimortalidade.Opresenteestudoavaliouseaclonidina,
夽 StudyconductedattheGraduatePrograminClinicalSurgery,HospitaldeClinicas,UniversidadeFederaldoParaná(UFPR).
∗Correspondingauthor.
E-mail:[email protected](C.G.R.Ferreira).
0104-0014/$–seefrontmatter©2014SociedadeBrasileiradeAnestesiologia.PublishedbyElsevierEditoraLtda.Allrightsreserved.
fármacodaclassedos␣-2agonistas,porviaraquidiana,semassociac¸ãocomanestésicoslocais ouopioides,reduzessarespostaemcirurgiascardíacascomusodecirculac¸ãoextracorpórea.
Método: Estudaram-se27pacientesentre18e75anos,separadosdemodonãoencobertoem grupocontrole(15)egrupoclonidina(12).Todosforamsubmetidosatécnicaidênticade aneste-siageral.Aseguir,apenasogrupoclonidinarecebeu1mg.kg−1declonidinaporviaraquidiana. Foramdosadososvaloresdeglicemia,lactatoecortisolemtrêstemposconsecutivos:T1,no momentodainstalac¸ãodapressãoarterialinvasiva (PAM);T2,dezminutos apósaprimeira dosedecardioplegia;eT3nasuturadapele,bemcomoosvaloresdetroponinaIemT1eT3. Avaliou-setambémavariac¸ãodosresultadosentre:T2-T1;T3-T2eT3-T1.
Resultados: Houve diferenc¸a estatisticamente significativa apenas quanto à variac¸ão da glicemianogrupoclonidina:T3-T2valordep=0,027eT3-T1valordep=0,047.
Conclusões:Aclonidinaespinhalemdosede1g.kg−1nãodiminuiuasdosagenssanguíneasde troponina,cortisoloulactato.Aglicemiasofreuumamenorvariac¸ãoduranteoprocedimento nogrupoclonidina.Essefato,járegistradonaliteratura,necessitademaioresinvestigac¸ões paraseresclarecido.
©2014SociedadeBrasileiradeAnestesiologia.PublicadoporElsevierEditoraLtda.Todosos direitosreservados.
Introduction
Surgical procedures induce an endocrine, metabolic and inflammatory response in the body that causes early and latechangesinhomeostasiswithproteincatabolism.These changesaredirectlyrelatedtotheintensityofthesurgical traumainduced.1
Althoughthissetofphysiologicalchangeshavea biolog-icalfunctiontofacilitatethehealingofinjuredtissuewhen theaggressionisintenseandprolonged,asoccursinmajor surgeries,theresponsetotraumabecomes,initself,acause ofincreasedmorbidityandmortality.2
Patients undergoing cardiac surgery with cardiopul-monarybypass(CPB)aresubjecttovariousformsof aggres-sion,suchastheexposureofbloodtothenon-physiological environment of CPB circuits, acute hemodilution and activationofthecoagulationcascadeand7thecomplement
system. As expected, many of these patients undergo intensephysiological changes thatmay persistfor several days.2,3 The systemicuseofhigh dosesofopioidsandthe
neuraxial blockade with a local anesthetic seem to be abletomodulatethisneuroendocrineresponsetosurgical stress. Both techniques, however, have their drawbacks, suchastherespiratorydepressionprolongedbyopioidsand thehypotensiontriggeredbyneuraxialblockade.4,5
Clonidine,adrugbelongingtotheclassof␣-2agonists,
has been associated with anesthetic-surgical procedures becauseof itsability to promote hemodynamic stability,6
toprolong the analgesia time of localanesthetics and to actinthe treatmentof postoperativepain.8,9In addition,
clonidinerevealed theabilitytomodulatetheresponseto surgicalstressandasignificantapplicationinthetreatment ofchronic pain.10---13 Somestudies also suggest that
cloni-dineacts toreduceperioperative morbidityandmortality inpatientsatriskforcoronarydisease.14,15
Numerousstudieshaveshownthatclonidine,when com-bined with local anesthetics and opioids by spinal route, playsarolepotentiatingtheiractions.However,spinal cloni-dine,assingledrug,hasbeenscarcelystudied.Thisresearch aims to assess the role of clonidine in the endocrine-metabolic stress response in adult patients undergoing
cardiacsurgerywithCPB,withtheuseoftroponinI,blood glucose,lactateandcortisolasmarkers.
Method
All patients underwent a similar technique for gen-eral anesthesia, with puncture of two peripheral veins, peripheral arterial catheter and induction of general anesthesia with etomidate 0.2---0.5mgkg−1 or propofol
1.0---2.5mgkg−1, fentanyl up to 5
gkg−1 and
pancuro-niumorvecuronium0.1mgkg−1.Maintenanceofanesthesia
wasperformed withfentanyl at amaximum total dose of 25gkg−1, distributedduringthe procedure,isofluraneat
a maximum concentration of 2.5% and repetition of neu-romuscular blocker asneeded. Vasoactive drugs could be used at any time at the discretion of the anesthesiolo-gist.
The study excluded patients with contraindications to spinal block,historyof acutemyocardial infarctionwithin thepastsixmonths,emergencysurgeryanduseof cortico-steroidsorclonidine.
Thepatientsallocatedtotheclonidinegroupwereplaced inlateraldecubituspositionandunderwentlumbarpuncture withdisposableneedle25GtypeQuincke,immediatelyafter trachealintubation.Assoonastheliquorflowedthroughthe needle,1gkg−1clonidinewasadministered,usinga1-mL
syringe.An interval of at least one hour between lumbar punctureandheparinadministrationwasobserved. Subse-quently,urinarycatheterizationandinstallationofacentral venouscatheterwereperformed.
Allpatients were monitored withcontinuous ECG with STsegmentanalysis,nasopharyngealtemperature,invasive blood pressure (MAP), capnography, pulseoximetry, urine output, blood gas,ventilatory monitoring withspirometry andgasanalysis.
3weremeasured.Wealsoassessedthevariationinresults betweenT2---T1,T3---T2andT3---T1.
CPB was performed with Braile Biomedica® or Nipro®
equipment, with oxygenators of the respective brands. For the infusion of blood from the CPB machine to the patient, Medtronic® or Terumo® centrifugal pumps were
used.ThroughouttheperiodofCPB,thetemperaturewas maintainedabove31◦C.
Parametric data were described as mean, median, standarddeviation,andminimumandmaximumvalues.The groupswerecomparedusingnon-parametricMann---Whitney test.p-Valueslowerthan0.05wereconsideredas statisti-callysignificant.
Results
Thestudyincluded27patients:15inthecontroland12in theclonidinegroup.Themeanagesofthecontrolgroupand oftheclonidinegroupwere52.53±13.10and51.75±14.75 years(p=0.885), respectively. The generalcharacteristics ofthegroupsareshowninTable1.
Table1 Generalcharacteristicsofgroups.
Control group(%)
Clonidine group(%)
Hypertension 60 67
Diabetes 13.30 16.70 Beta-blocker 60 33.30 Valvesurgery 40 75.00 Coronarysurgery 60 25
Thegroupswerehomogenousintermsofejection frac-tion, fractional shortening percentage, plasma creatinine anddurationofCPB(Table2).
Plasmacortisolvaluesincontrolandclonidinegroupsare showninTable3.
BloodglucosevaluesareshowninTable4.
Table5displaysserumlactatevaluesinbothgroups. TroponinvaluesforthetwogroupsareshowninTable6. There was no statistical difference at the significance levelof5% forblood levelsoftroponin I,lactate,glucose andcortisolinalltimesanalyzedinisolation.Therewasa
Table2 Serumcreatinine,PS(%),EF(%)andCPBtimeinbothgroups.
Controlgroup Clonidinegroup p-Value
Creatinine(mg/dL) 1.15±0.38 1.09±0.28 0.684
PS(%) 34.52±8.39 33.43±9.75 0.762
EF(%) 58.81±14.45 60.67±13.68 0.737
CPB(min) 92.27±23.53 78.75±37.13 0.260
PS,percentualshortening;EF,ejectionfraction;CPB,cardiopulmonarybypass.
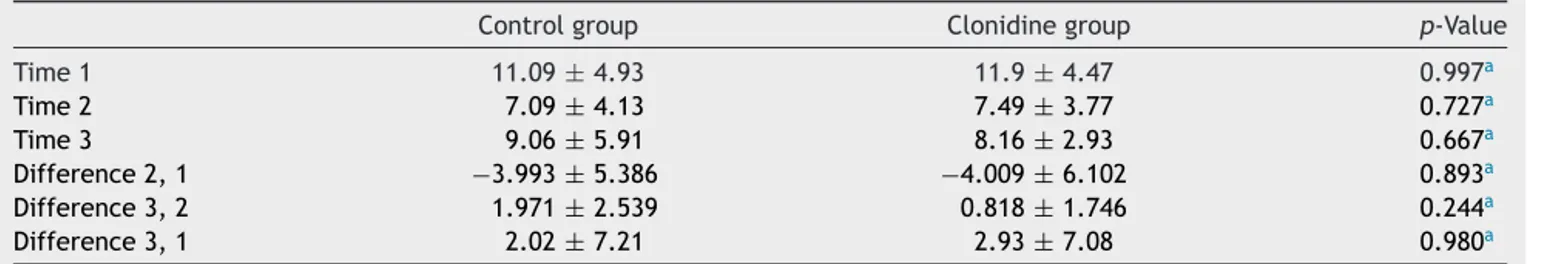
Table3 Serumcortisol(g/dL)atTimes1,2and3(mean±standarddeviation).
Controlgroup Clonidinegroup p-Value
Time1 11.09±4.93 11.9±4.47 0.997a
Time2 7.09±4.13 7.49±3.77 0.727a
Time3 9.06±5.91 8.16±2.93 0.667a
Difference2,1 −3.993±5.386 −4.009±6.102 0.893a
Difference3,2 1.971±2.539 0.818±1.746 0.244a
Difference3,1 2.02±7.21 2.93±7.08 0.980a
Time1,punctureforPAMmonitoring;Time2,10minafterfirstcardioplegia;Time3,skinsuture.
a Withoutstatisticalsignificance.
Table4 Bloodglucose(mg/dL)atTimes1,2and3(mean±standarddeviation).
Controlgroup Clonidinegroup p-Value
Time1 101.4±12.84 109.75±24.42 0.615a
Time2 154.4±48.69 150.64±22.1 0.919a
Time3 176.13±57.38 146.67±36.7 0.126a
Difference2,1 53±39.86 39.821±23.63 0.433a
Difference3,2 21.73±25.14 −2.83±29.13 0.027b
Difference3,1 74.73±48.41 36.92±17.49 0.047b
Time1,punctureforPAMmonitoring;Time2,10minafterfirstcardioplegia;Time3,skinsuture.
a Withoutstatisticalsignificance.
Table5 Determinationofserumlactate(mg/dL)atTimes1,2and3(mean±standarddeviation).
Controlgroup Clonidinegroup p-Value
Time1 1.35±0.55 1.68±0.56 0.152a
Time2 2.8±0.98 2.64±1.19 0.702a
Time3 3.29±1.39 3.16±1.78 0.719a
Difference2,1 1.446±0.947 0.895±1 0.077a
Difference3,2 0.485±0.901 0.605±1 0.0761a
Difference3,1 1.931±1.312 1.487±1.715 0.126a
Time1,punctureforPAMmonitoring;Time2,10minafterfirstcardioplegia;Time3,skinsuture.
aWithoutstatisticalsignificance.
Table6 DeterminationoftroponinI(/dL)atTimes1and3(mean±standarddeviation).
Controlgroup Clonidinegroup p-Value
Time1 0.021±0.04 0.039±0.072 0.399a
Time3 1.571±2.289 1.575±1.636 0.236a
Time3,1 1.550±2.298 1.536±1.657 0.299a
Time1,punctureforPAMmonitoring;Time3,skinsuture.
aWithoutstatisticalsignificance.
statisticallysignificantdifferenceinbloodglucosevariation attimesT3---T2(p=0.027)andT3---T1(p=0.047).
Discussion
Thepresentstudyevaluatedtheeffectsofspinalclonidine onsurgical stress responsein patients undergoingcardiac surgerywithCPB.Thesurgicaltraumaresponseisformedby complexhormonalandmetabolic changesthatprofoundly alterhomeostasisandparticipateinthemorbidityand mor-talityobservedinmediumandmajorsurgeries.
Theuseofneuraxialclonidineinhumansbeganin1984.16
Sincethen,numerous studiessuggestthatspinalclonidine potentiatestheeffectsofopioidsandlocalanesthetics.7,13
Therefore,whenthisassociationoccurs,itmaybedifficult toseparatetheeffects producedonlybyclonidine.Spinal clonidinenotassociatedwithotherdrugsorotherformsof anesthesiawastheobjectofanalysisinagroupofobstetric patients.The patients were randomlyassigned toreceive either 50, 100 or 200g of subarachnoidclonidine in the
firststageof labor.Theresultsindicatethatclonidinehas an analgesic action in the spinal cord.The authors point outthatthedoseof100goffersthebestdose-sideeffects
relation.17
Itisknownthattheactionofspinalclonidineismediated bytheactivationof␣-2receptorsinthesubstantia
gelati-nosa,withblockage of potassium conductance offibers C andA.18,19Thedrugalsoactsinthelocuscoeruleusby
reduc-ingthecentralreleaseofnorepinephrine,withattenuation of the central sympatheticaction.16,20 Both actions could
occurwithintrathecal clonidine, whichwould actboth in thedorsalhornofthespinalcordandinthelocuscoeruleus
aftermigrating, throughthe liquorto thehigher centers. Thereis,therefore,atheoreticalbasistojustifyaprotective actionofclonidineonstressresponses.
Troponin I, cortisol, glucose and lactic acid were the markersusedinthisstudytoidentifystressresponsesand
theirmodificationsbytheinterventionofclonidine.These markershavealreadybeenextensivelyvalidatedinprevious studies.21---26
Inthepresentstudy onlybloodglucoseexhibitedmore moderateelevationinthegroupreceivingspinalclonidine. This suggeststhat somehow therewas a lower activation ofstressin thisgroup.Onecannotsaythatthisglycaemic changehasclinicalsignificance,althoughwithstatistical sig-nificance.Thus,thereisnosufficientevidencetocontend thatclonidinehasaprotectiveroleinstress,whenusedby spinalroute.
Conclusion
There were no statistically significant differences in tro-poninI,cortisolorlacticaciddeterminationsbetweenthe groups. Blood glucose showed a more moderate increase in the group receivingspinal clonidine. We conclude that the use of clonidine at the spinal dose of 1gkg−1 was
not able to reduce the intensity of response to surgical trauma and showed only modest activity on glucose lev-els.
Conflicts
of
interest
Theauthorsdeclarenoconflictsofinterest.
References
1.DesboroughJP.Thestressresponsetotraumaandsurgery.BrJ Anaesth.2000;85:109---17.
2.Warren OJ, Smith AJ, Alexiou C, et al. The inflammatory responsetocardiopulmonarybypass:part1---mechanismsof pathogenesis.JCardiothoracVascAnesth.2009;23:223---31.
4.ChaneyM.Intrathecalandepiduralanesthesiaandanalgesiafor cardiacsurgery.AnesthAnalg.2006;102:45---64.
5.Suleiman M-S, Zacharowsk K, Angelini GD. Inflammatory responseandcardioprotectionduringopen-heartsurgery:the importanceofanaesthetics.BrJPharmacol.2008;153:21---33.
6.WatanabeT,InagakiY,IshibeY.Clonidinepremedicationeffects on inhaled induction with sevoflurane in adults: a prospec-tive,double-blind,randomizedstudy.ActaAnesthesiolScand. 2006;50:180---7.
7.Elia N, Culebras X, Mazza C, et al. Clonidine and adju-vant to intrathecal localanesthetics for surgery: systematic reviewof randomizedtrials. RegAnesth Pain Med. 2008;33: 159---67.
8.LenaP,BalaracN, ArnulfJ,et al. Intrathecalmorphineand clonidinefor coronary arterybypass grafting. Br J Anaesth. 2003;90:300---3.
9.Nader D, Li CM, Dosluoglu HH, et al. Adjuvant therapy with intrathecal clonidine improves postoperative pain in patientsundergoingcoronaryarterybypassgraft.ClinJPain. 2009;25:101---6.
10.Morin AM, Geldner G, Schwarz U, et al. Factors
influenc-ing preoperative stress response in coronary artery bypass
graft patients. BMC Anesthesiol. 2004;4:7. Available from
http://www.biomedcentral.com/1471-2253/4/7
11.Schneemilch C, Bachmann H, Elwert R, et al. Clonidine decreases stress response in patients undergoing carotid endarterectomyunderregionalanesthesia:aprospective, ran-domized, double-blinded, placebo-controlled study. Anesth Analg.2006;103:297---302.
12.GrosuI, Kock M. New conceptsin acute pain management: strategies to prevent chronic postsurgical pain, opioid-inducedhyperalgesia,andoutcomemeasures.AnesthesiolClin. 2011;29:311---27.
13.GiovannoniMP,GhelardiniC,VergelliC,etal.␣2agonistsas analgesicagents.MedResRev.2009;29:339---68.
14.WallaceAW, Galindez D, Salahieh A, et al. Effect of cloni-dineoncardiovascularmorbidityandmortalityafternoncardiac surgery.Anesthesiology.2004;101:284---93.
15.NishinaK,MikawaK,UesugiT,etal.Efficacyofclonidinefor pre-ventionofperioperativemyocardialisquemia.Anesthesiology. 2002;96:323---9.
16.Eisenach JC, DeKock KM, Klimscha W. Alpha sub2 adrener-gic for regional anesthesia a clinicalreview. Anesthesiology. 1996;85:655---74.
17.Chiari A, LorberC, EisenachJC, et al. Analgesicand hemo-dynamiceffectsofintrathecalclonidineasthesoleanalgesic agentduringfirststageoflabor:adoseresponsestudy. Anes-thesiology.1999;91:388---96.
18.Reddy SVR, Yaksh TL. Spinal noradrenergic terminal system mediatesantinociception.BrainRes.1980;189:391---401.
19.Brandt SA, Livingston A. Receptor changes in spinal cord of sheep associated with exposure to chronic pain. Pain. 1990;42:323---39.
20.WallaceAW.Clonidineandmodificationofperioperative out-come.CurrOpinAnaesthesiol.2006;19:411---7.
21.Lehrke M,BroedlUC, Biller-FriedmannIM, etal.Serum
con-centrationsofcortisol,interleukin 6,leptin,andadiponectin
predict stress induced insulin resentence in acute
inflam-matory reactions. Crit Care. 2008;12:R157. Available from
http://ccforum.com/content/12/6/R157
22.LattermannR,SchrickerT,GeorgieffM,etal.Lowdose cloni-dinepremedicationaccentuatesthehyperglycemicresponseto surgery.CanJAnaesth.2001;48:755---9.
23.ChiS, SteinE,ChaneyM,etal.Severelacticduringcardiac surgery.JCardiothoracVascAnesth.2009;23:711---9.
24.BarryJAW, BarthJH,HowellSJ.Cardiac troponins:theiruse andrelevanceinanaesthesiaandcriticalcaremedicine.Contin EducAnaesthCritCarePain.2008;8:62---6.
25.DeverauxPJ. Can attenuationof theperioperative response prevent intermediate or long-term cardiovascular outcomes amongpatientsundergoingnoncardiacsurgery?Anesthesiology. 2009;111:223---6.